Obesity is a risk factor for many chronic diseases that contribute significantly to health care spending in the United States. In this chart collection, we explore the costs associated with obesity for people with large employer private insurance. We use data from the Merative MarketScan Commercial Database from 2011 through 2021.
We find that, on average, privately insured people with an obesity diagnosis have higher total and out-of-pocket spending than people without an obesity diagnosis. We also look at the cost of common surgical and pharmacological treatments for obesity. We find that inpatient bariatric surgeries cost $32,868, on average, in 2021.
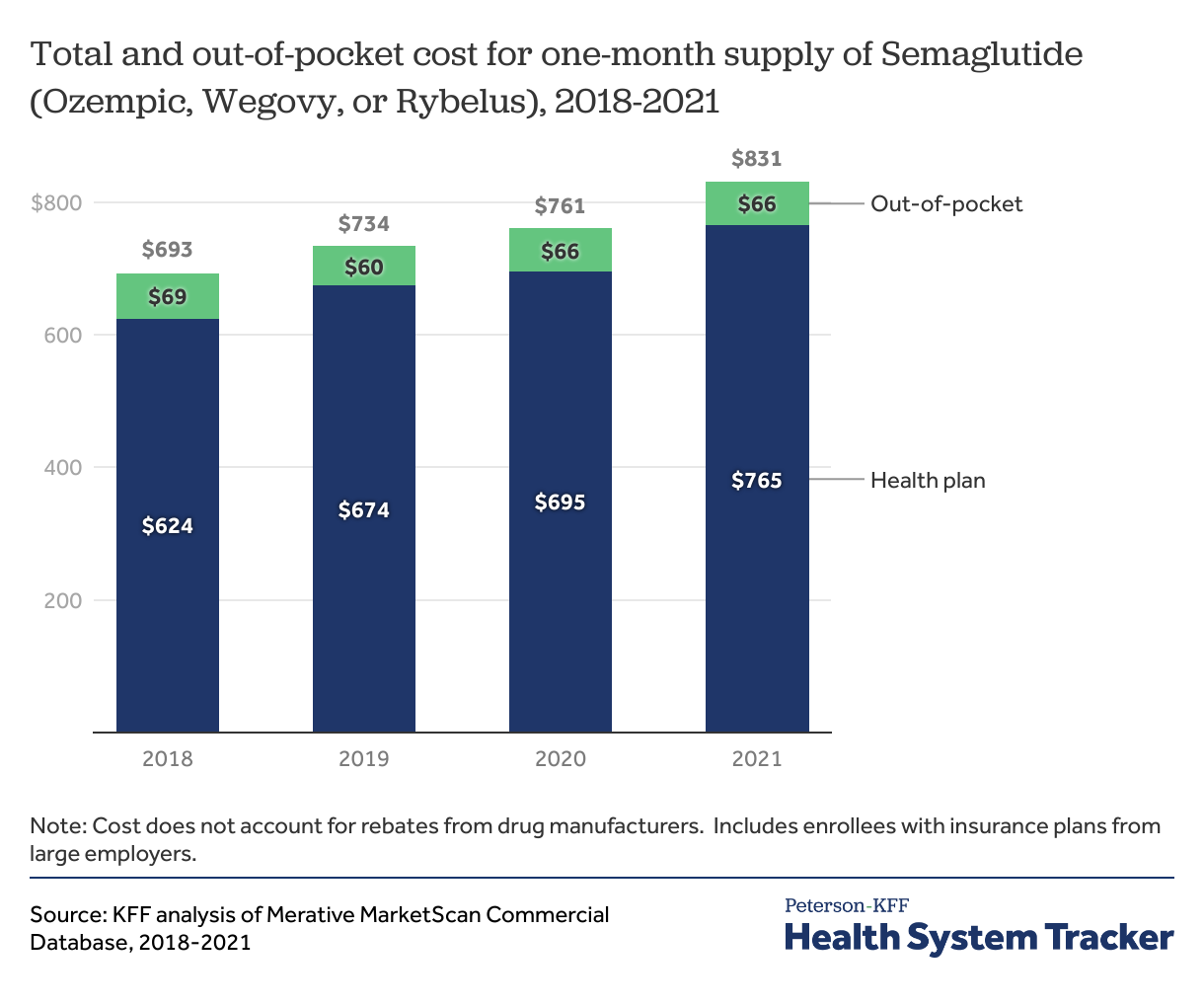
Recently, the FDA approved Wegovy for weight loss, which is a new formulation of the diabetes drug Ozempic (Semaglutide). We find the average Semaglutide prescription cost $831 per month in 2021 (not accounting for rebates), and consumers paid $66 out-of-pocket per month, on average. The monthly total cost of Semaglutide has increased 20% since it came to market in 2018, though we are unable to account for rebates that may be offsetting these costs.
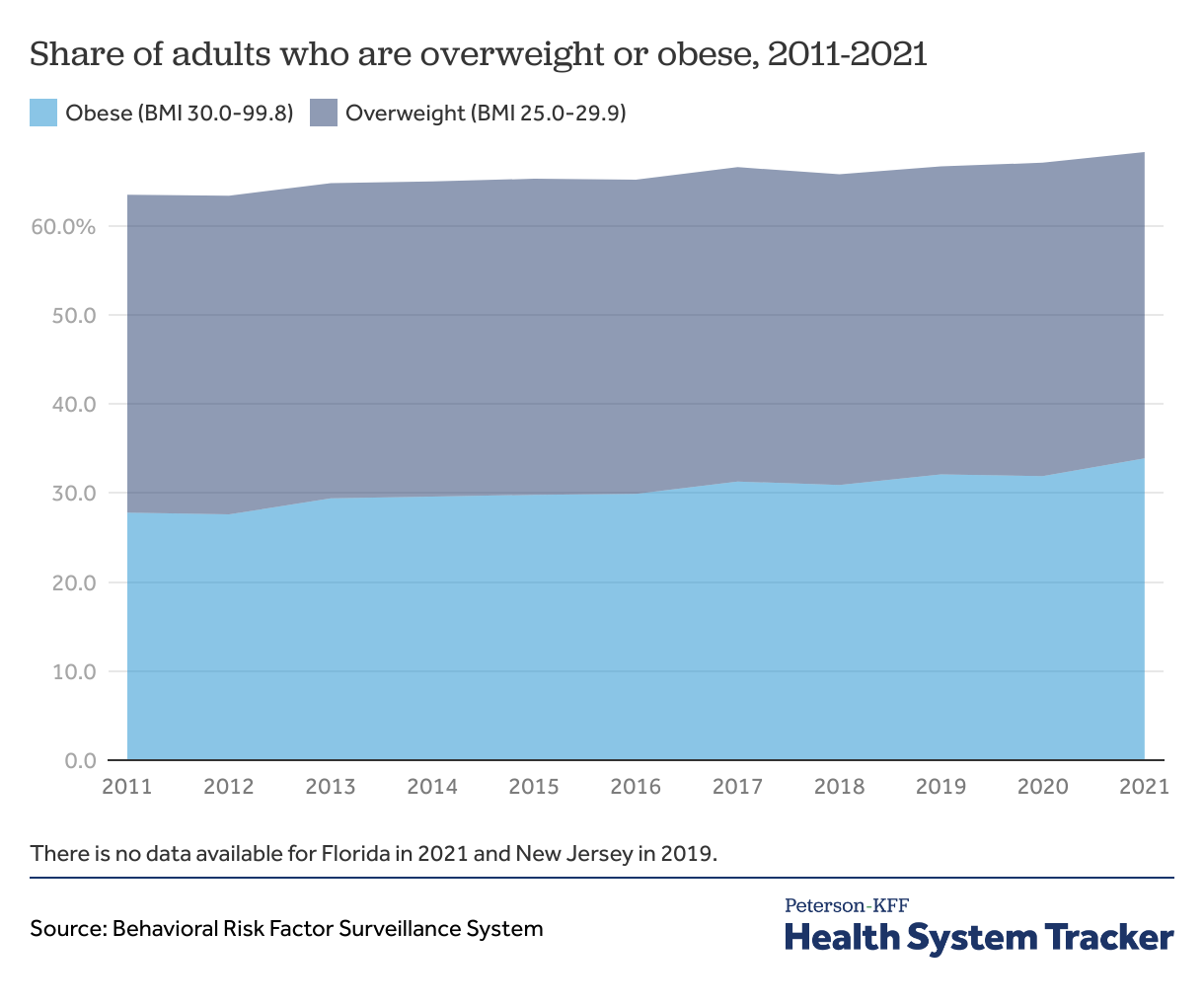
Rates of obesity in the U.S have increased over time
In the United States, the share of adults who are obese has increased over time. While the share of people who are overweight but not obese has remained relatively stable since 2011, the share of people with obesity increased from 28% in 2011 to 34% in 2021. In addition to the biological underlying causes of obesity, numerous structural factors also contribute to obesity, including stress, food insecurity, and lack of time for and access to leisure and recreation.
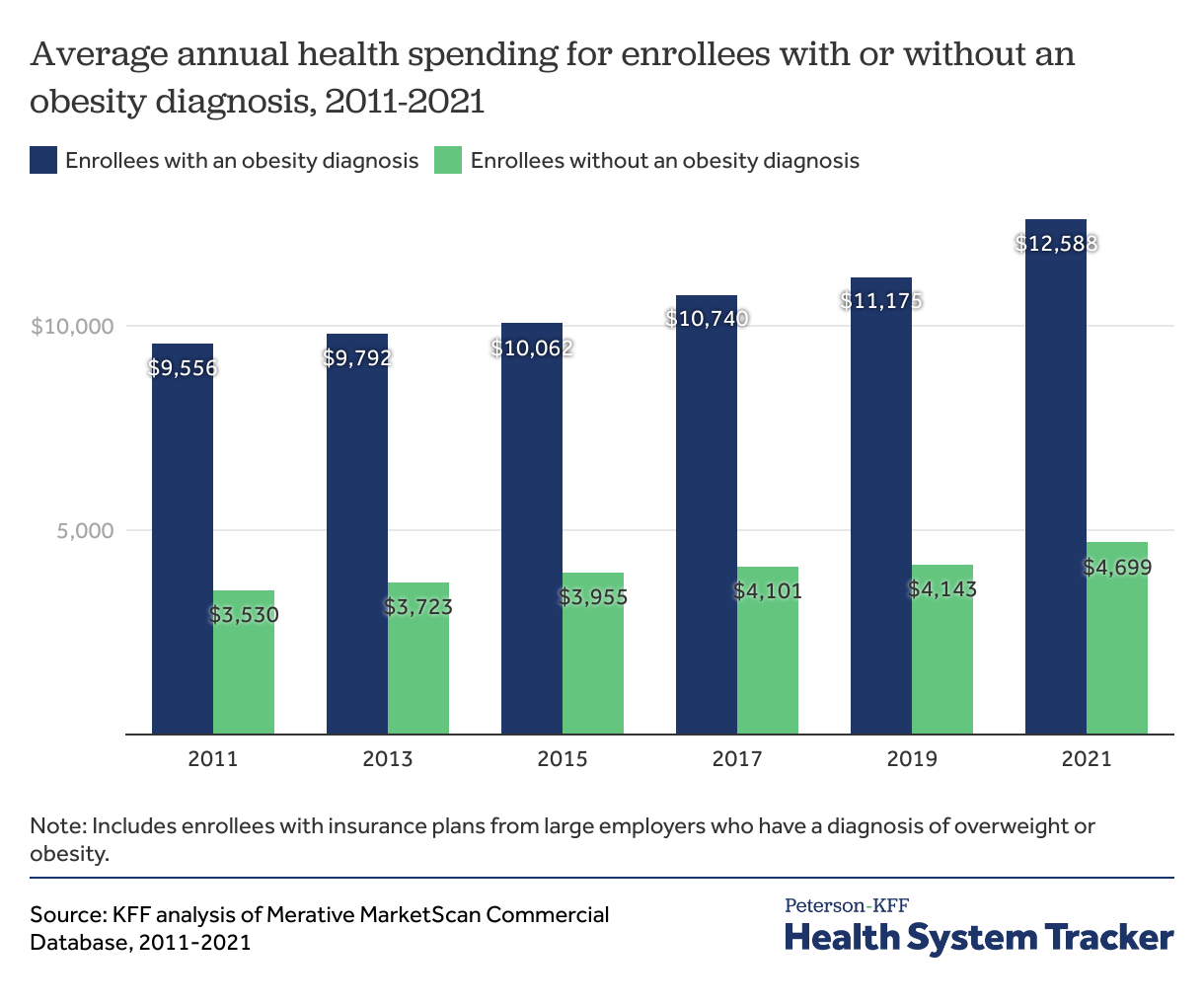
Enrollees with obesity and overweight diagnoses have higher health spending than those without such diagnoses
In 2021, people with large employer private insurance coverage who had an obesity or overweight diagnosis had an average of $12,588 in total annual health costs, which is more than double the $4,699 in health spending for those with no obesity or overweight diagnosis on their health insurance claims for that year.
On average, total spending for privately insured people with an obesity or overweight diagnosis increased 32% over the past ten years, similar to the increase of 33% for those without an obesity or overweight diagnosis.
People with obesity may have higher health costs for a variety of reasons. As obesity often coincides with chronic health conditions, annual costs for people with obesity capture both direct costs of treating obesity as well as spending on other health conditions in that same year. This might include costs for treatments of obesity (such as bariatric surgery or pharmacologic therapy, discussed below), as well as treatments of other conditions that are caused by or worsened by weight. Obesity often also co-occurs with several other disorders including high cholesterol, hypertension, and elevated blood sugar (the so-called “metabolic syndrome”). These conditions also increase risk for numerous chronic diseases including cardiovascular disease, stroke, liver disease, osteoarthritis, and even some types of cancer.
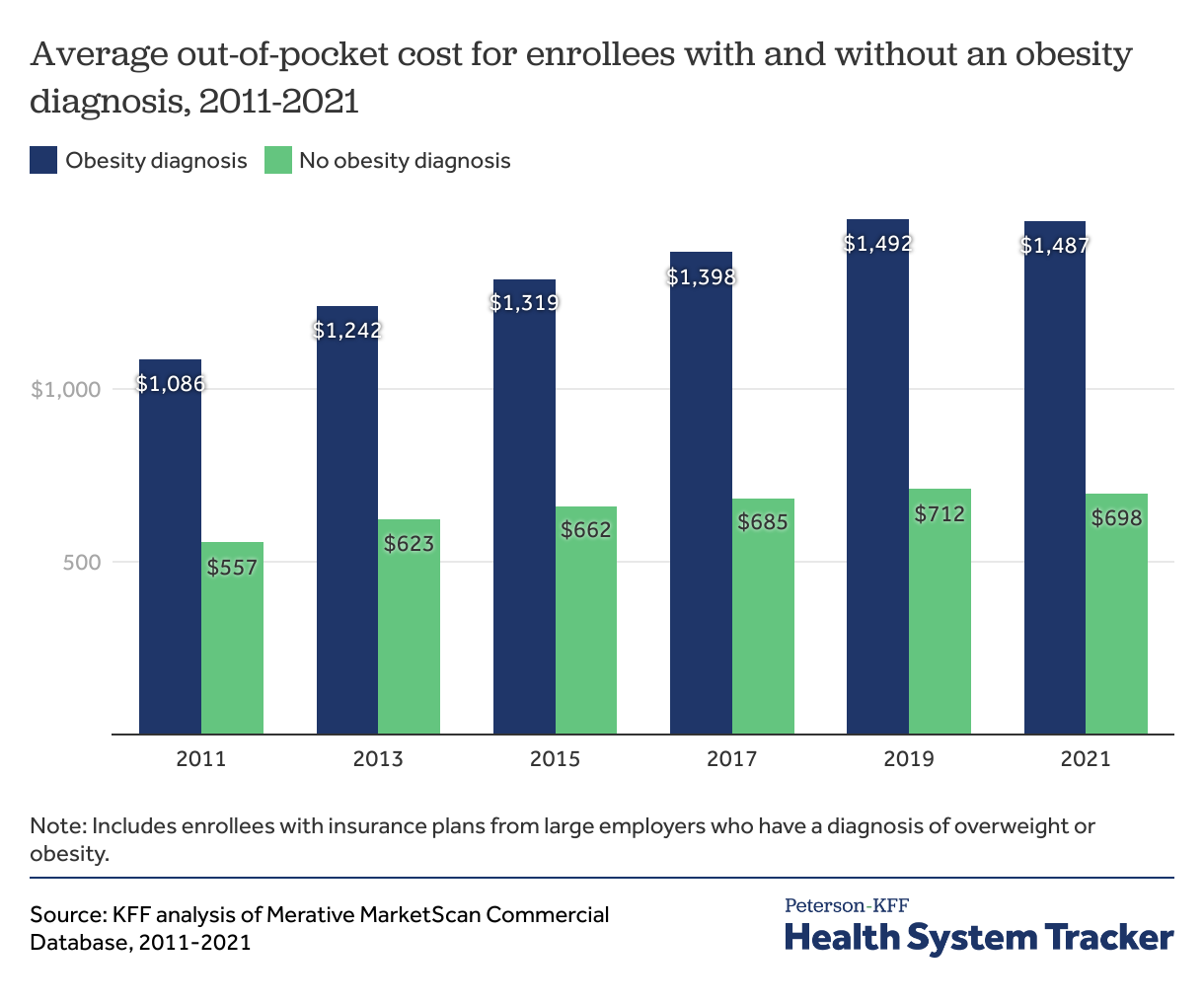
Enrollees with obesity or overweight diagnoses have had faster growth in out-of-pocket costs than those without such diagnoses
People with obesity or overweight diagnoses have higher out-of-pocket costs than those without such diagnoses. In 2021, people with large employer coverage who had an obesity diagnosis faced an average of $1,487 in out-of-pocket costs, compared to $698 for those without an obesity diagnosis.
Out-of-pocket spending has grown more quickly for people with obesity than for those without an obesity diagnosis on their record. On average, out-of-pocket costs have increased 37% over the last decade for people with large employer coverage who have an obesity diagnosis, compared to an increase of 25% for those without such diagnosis.
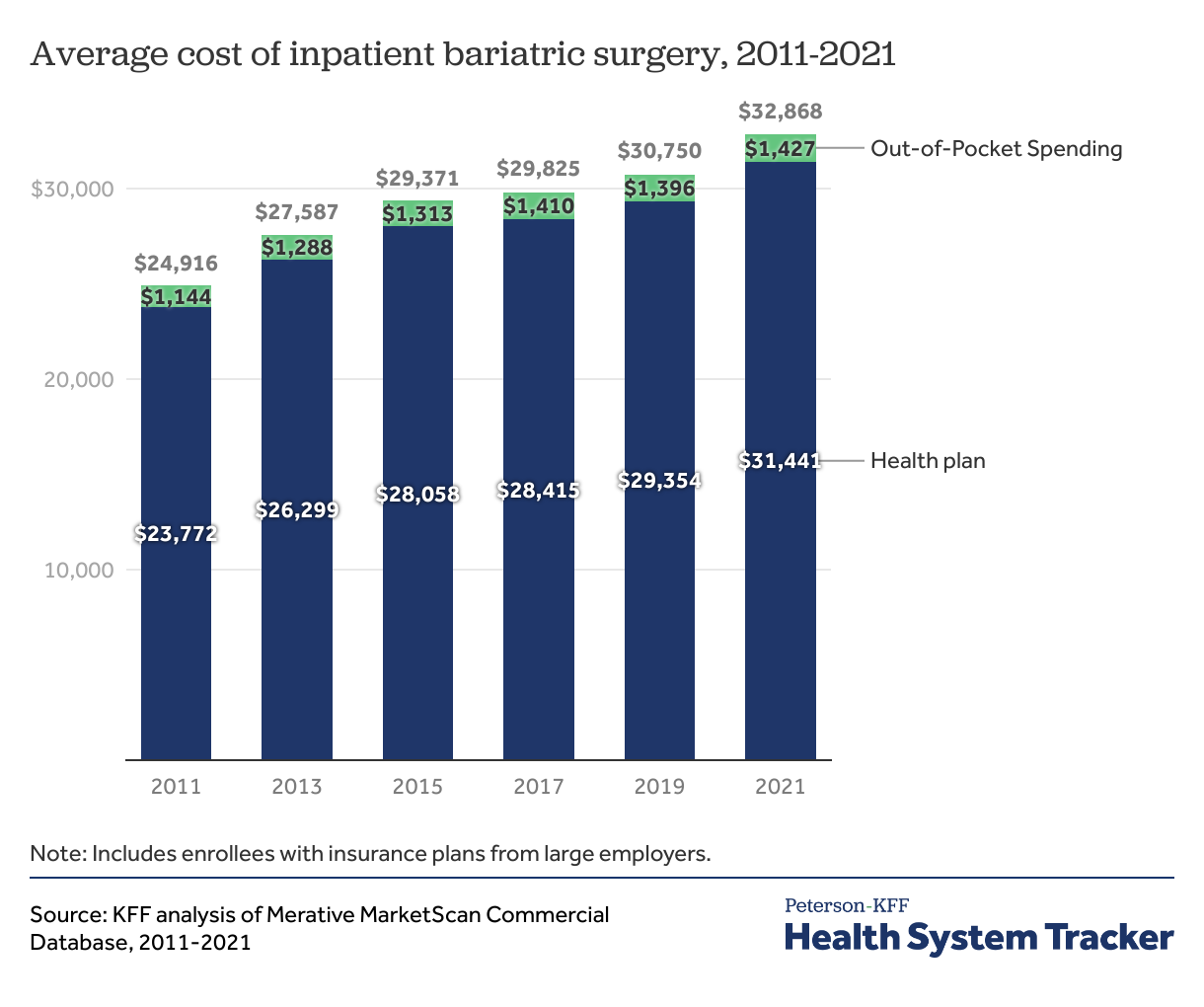
Inpatient bariatric surgeries are more common, and more expensive, than outpatient surgeries
One treatment for obesity is bariatric surgery, which is a group of surgeries that assists with weight loss for people with a high BMI. While bariatric surgery has positive long-term benefits in many patients, uptake of the procedure is historically low due to several barriers including provider and patient knowledge and attitudes, access to care, and cost.
In 2021, the large majority (86%) of bariatric surgeries occurred in the inpatient setting. The average inpatient bariatric surgery cost $32,868, including the amount paid by the health plan and out-of-pocket by the enrollee through the health plan. The cost of inpatient bariatric surgery has risen over the past decade. The total cost of inpatient bariatric surgery increased 32%, from $24,916 in 2011 to $32,868 in 2021, on average. There was also significant variation in costs, with a quarter of inpatient surgeries costing less than $24,645 and a quarter costing more than $37,510, on average. The most expensive 10% of inpatient surgeries cost over $49,905.
People with large employer coverage receiving bariatric surgery paid an average of $1,427 out-of-pocket for inpatient surgeries in 2021. For people with large employer coverage, average out-of-pocket costs associated with inpatient bariatric surgery increased 24%, from $1,144 in 2011 to $1,427 in 2021. Though this is an average across both in-network and out-of-network care, these out-of-pocket costs do not reflect any balance billing consumers may face from out-of-network providers. In 2021, a quarter of bariatric surgery patients with large employer health coverage paid more than $2,268 out-of-pocket for their surgeries.
A number of enrollees in large employer health plans had no out-of-pocket costs associated with their bariatric surgery, though they may have already reached their deductible or out-of-pocket maximum before having the surgery. Because people with obesity diagnoses tend to have higher health spending and out-of-pocket costs generally, and because bariatric surgery requires extensive pre-operative testing and care, people receiving bariatric surgery may be more likely to reach their deductible or out-of-pocket maximum in a given year.
The cost of inpatient bariatric surgery has risen over the past decade. The total cost of inpatient bariatric surgery increased 32%, from $24,916 in 2011 to $32,868 in 2021, on average. Average out-of-pocket costs increased 25%, from $1,144 in 2011 to $1,427 in 2021.
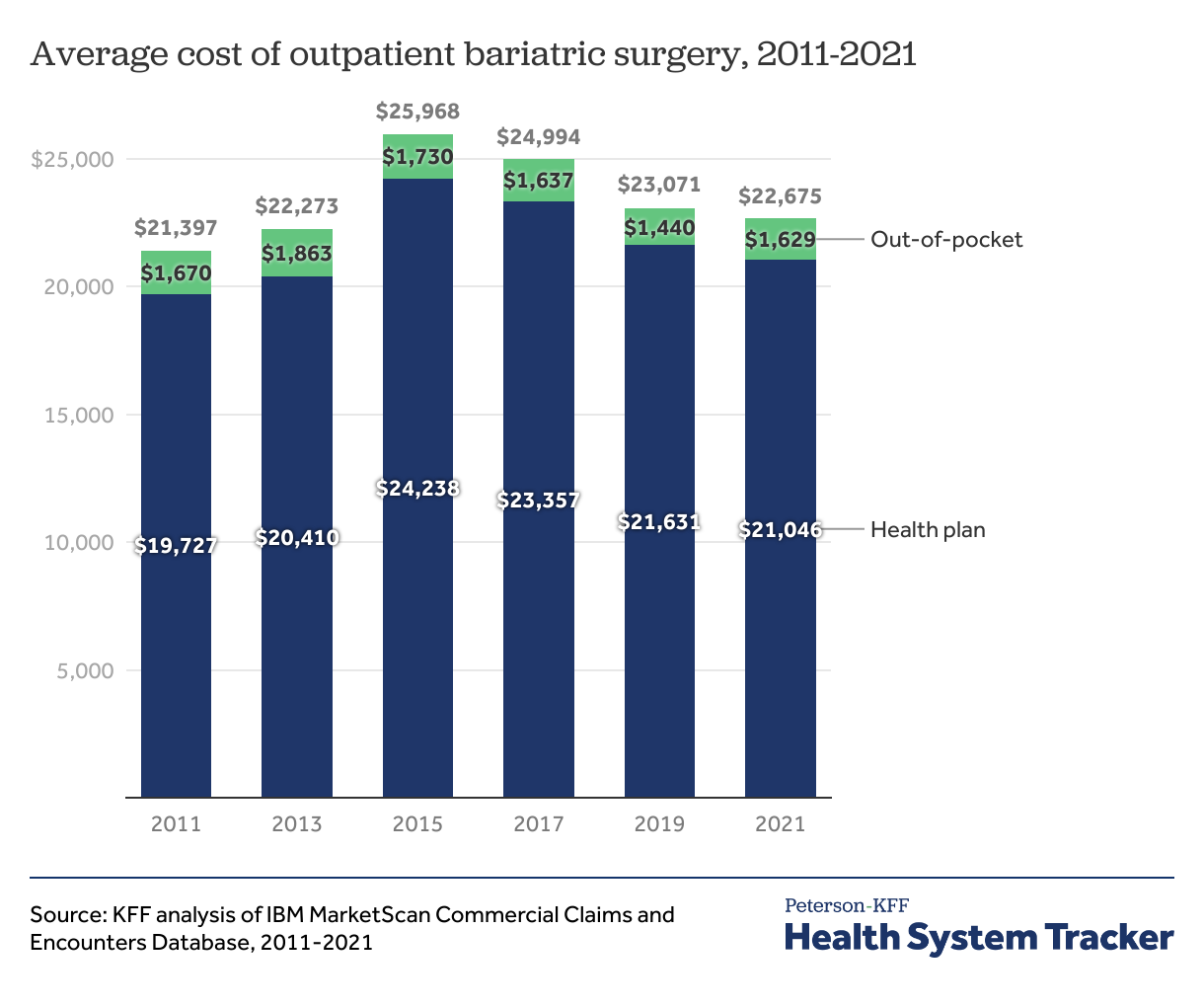
Outpatient bariatric surgeries have higher out-of-pocket costs than inpatient surgeries
In 2021, 14% of bariatric surgeries were outpatient. The average outpatient bariatric surgery cost $22,675, or $7,662 less than the average inpatient surgery. A quarter of outpatient surgeries cost more than $28,572, and the most expensive 10% cost more than $38,256.
Consumers paid $1,629 out-of-pocket, on average, for outpatient bariatric surgery in 2021, which is $166 more than the average inpatient bariatric surgery. The most expensive quarter of surgeries cost consumers over $2,437, on average, in 2021, and the most expensive 10% of surgeries cost over $3,828 out-of-pocket.
The cost of Semaglutide has increased, not accounting for rebates
In 2021, the FDA approved a new formulation of a once-weekly injectable diabetes drug Semaglutide for weight loss (Wegovy). Clinical trial data for Semaglutide showed greater reduction in BMI compared to prior weight loss drugs. Semaglutide has been on the market since approval in 2017 as the weekly injectable Ozempic and since 2019 as the oral formulation Rybelsus. While both are indicated for diabetes management, Ozempic has often been used off-label for weight loss for people without diabetes.
We look at all prescriptions for a one-month supply of Semaglutide since 2018 (for any diagnosis or dose) and find that, for enrollees with Semaglutide prescriptions in 2021, the cost for a one-month supply was $831, on average. There was limited variation in the total cost of a one-month supply, with half of prescriptions costing between $807 and $838 in 2021. However, we are unable to account for rebates paid by drug manufacturers, so the cost paid by health plans may actually be lower. The monthly cost of Semaglutide prescriptions increased 20% from 2018 to 2021, not including rebates.
Enrollees paid $66 out-of-pocket, on average, in 2021 for a one-month supply of Semaglutide. A quarter of prescriptions cost less than $15 out-of-pocket, on average, and another quarter cost more than $80 out-of-pocket, on average. These costs are averaged over all months in the year, and some people taking Semaglutide may reach their deductible or out-of-pocket maximum mid-year.
Methods
This analysis is based on data from the Merative MarketScan Commercial Database, which contains claims information provided by a sample of large employer plans. We used claims from 2011-2021. In 2021, there were claims for over 13 million of the 85 million people in the large group market. To make MarketScan data representative of large group plans, weights were applied to match counts in the Current Population Survey for enrollees at firms of a thousand or more workers by sex, age and state. Adults less than 65 years old with continuous enrollment in their plan for at least 6 months were included.
Annual spending, inpatient admission costs, and prescription costs were included if they were between $0 and the 99.5th percentile of cost. Total spending is the sum of the amount paid by the insurer and the amount paid by the enrollee. Out-of-pocket expenses are a sum of coinsurance, copays, and deductibles where applicable. The MarketScan database includes only claims covered by the enrollees’ plan and does not include any balance billing directly from providers to enrollees.
Midway through 2015, MarketScan claims transitioned from ICD-9 to ICD-10. While both systems classify diagnoses and procedures, they do not precisely crosswalk. Diagnosis and procedure codes in ICD-9 and ICD-10, as well as Current Procedural Terminology (CPT) codes for procedures, were selected based on a review of the relevant literature. Medications were identified using the National Drug Code (NDC) numbers maintained by the FDA.
Below is a summary of codes were included in each measure:
- Obesity or overweight diagnosis was defined as present if an enrollee had inpatient or outpatient services claims during the year with any diagnosis of ICD-10 code E66 or ICD-9 code 2780.
- The cost of an inpatient admission for bariatric surgery was defined as the sum of all services associated with an inpatient admission with a diagnosis of overweight or obesity, and with one of the following CPT codes: 43644, 43645, 43770, 43775, 43845, 43846, 43847.
- The cost of an outpatient bariatric surgery was defined as the sum of all outpatient services on a day with a bariatric surgery CPT code (43644, 43645, 43770, 43775, 43845, 43846, 43847), an anesthesia CPT code, and a facility fee of at least $1,500.
- Semaglutide prescriptions included all NDCs for all formulations of Semaglutide including the injectable formulations Ozempic (since 2018) and Wegovy (since 2021) and the oral formulation Rybelsus (since 2019). Prescriptions for a one-month supply were included when the days supplied was either 28 or 30 days.
The Peterson Center on Healthcare and KFF are partnering to monitor how well the U.S. healthcare system is performing in terms of quality and cost.