Earlier this year we released an analysis looking at how often health plans had taken steps to limit out-of-pocket costs for their enrollees during the pandemic. We found that many individual and fully-insured group market insurers had waived cost-sharing (copays, coinsurance, or payments towards a deductible) for patients receiving treatment for COVID-19 at some point during the pandemic. These waivers covered a combined 88% of enrollees in both markets at some point during the pandemic. However, at the time of our last analysis, some waivers had already expired and many more were set to expire in the fall. At the time, we also found that a small number insurers across both markets had extended some form of premium relief to their enrollees, most often in the form of a premium credit or rebate.
As the year has progressed, more data has become available to suggest that insurers have been quite profitable during the pandemic. Overall healthcare utilization and spending rapidly declined through the first half of the year as consumers delayed elective or non-emergency care, leaving many insurers with far more premium income than claims costs. Under the Affordable Care Act’s (ACA) Medical Loss Ratio (MLR) rule, insurers must spend a certain amount of their premium income on health care costs for their enrollees or pay back any excess profits to consumers in the form of rebates the following year. As of June 2020, KFF analysis found that individual and fully-insured group market insurers were on track to owe substantial rebates to consumers based on their margins and medical loss ratios this year, and even though there are some indications that healthcare utilization was returning to more normal levels, rising numbers of COVID-19 cases across the country may cause healthcare utilization and spending to decrease yet again this fall and winter.
In this brief, we reevaluate the number of enrollees whose insurer has waived cost-sharing for COVID-19 treatment at some point during the pandemic, as well as when these waivers are set to expire, to see how many insurers had extended the waivers beyond their earlier expiration dates, based on the trajectory of the pandemic and their financial performance. We also re-examine how many enrollees have been offered some form of premium credit or reduction thus far. We had previously speculated that insurers were issuing cost-sharing waivers and premium credits to increase their claims costs relative to their premium income in order to pre-empt massive MLR rebates they may owe next year. We find that, due to insurers delaying expiration dates, plans covering 71% of enrollees in all fully-insured commercial markets continue to have COVID-19 treatment cost waivers in place at this time. Additionally, plans covering 40% of enrollees in these markets have offered some form of premium relief.
We reviewed an updated summary of private insurers’ responses to the pandemic compiled by America’s Health Insurance Plans (AHIP). We systematically collected data from this summary and merged it onto enrollment data from Mark Farrah Associates TM in order to estimate how many individual and fully-insured group market enrollees are in plans that have waived cost-sharing for COVID-19 treatment or are offering some form of premium relief.
Importantly, our estimates do not include the substantial portion (61%) of the group market enrolled in self-insured employer plans. These plans are established and funded by an employer and are not always subject to federal regulation. As such, the benefit designs of these plans, including the services that they opt to cover and any associated cost-sharing, are left to the discretion of the employer. There is no source of comprehensive data on the prevalence of these policies and, therefore, they are not included in this analysis.
Cost-sharing waivers for COVID-19 treatment
Federal legislation still requires that all private insurance plans, including self-funded plans, cover the entire cost associated with approved COVID-19 testing so long as the test is deemed medically appropriate. However, there are still no provisions that require private insurers to waive cost-sharing for COVID-19 treatment, such as hospitalizations. Only five states (MA, NM, ID, MI, MN) and D.C. require or have agreements in place with insurers to waive out-of-pocket treatment costs for their fully-insured plan enrollees, although, as this analysis finds, many insurers continue to voluntarily waive out-of-pocket costs for enrollees who require COVID-19-related treatment.
Most fully-insured enrollees are in plans that waived cost-sharing for COVID-19 treatment and many plans have postponed their waiver’s expiration date since July
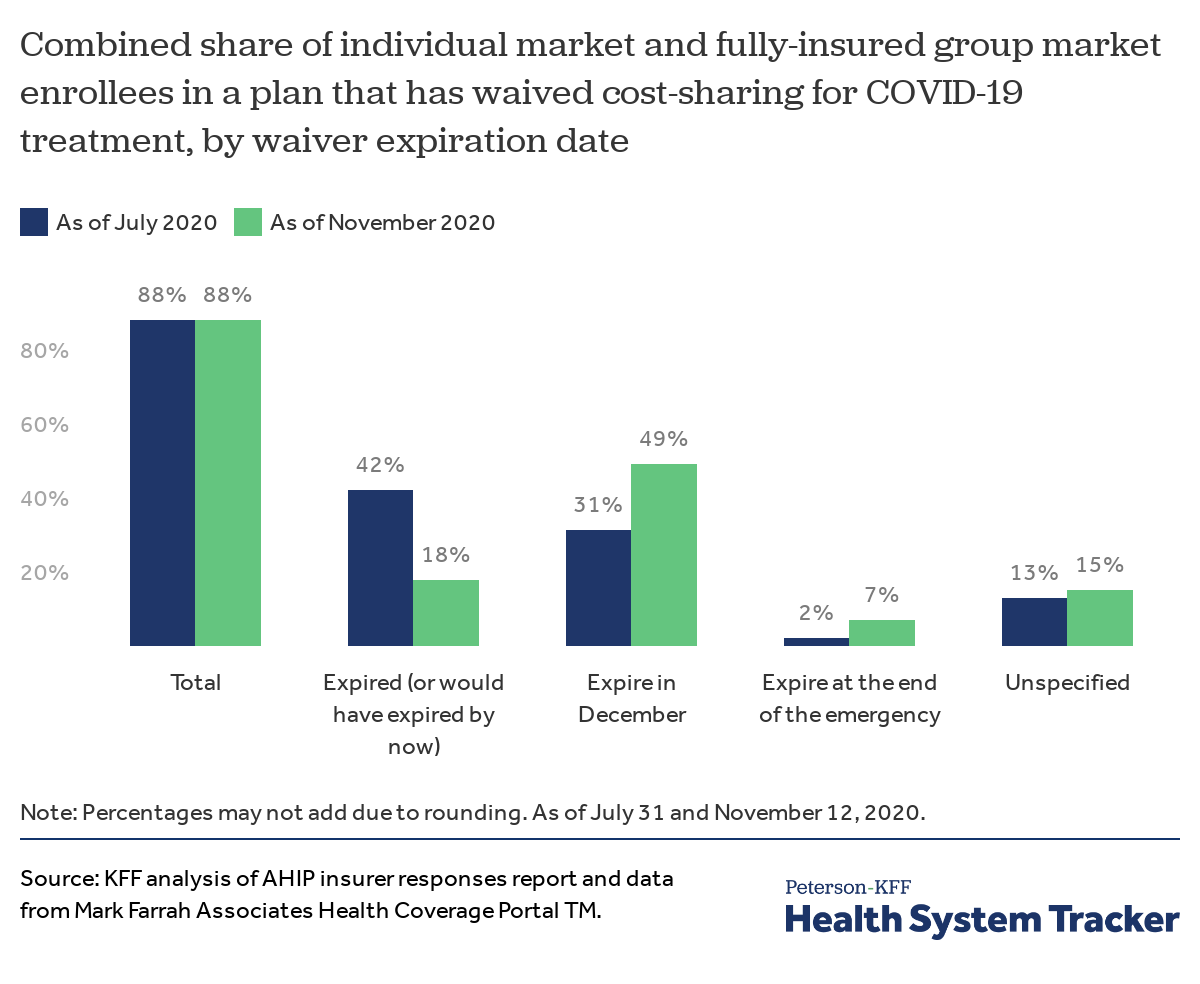
Across all individual and fully-insured group plans, 88% of enrollees are in a plan that has at some point during the pandemic waived out-of-pocket costs for COVID-19 treatment, the same share as when we initially checked in late July. Of these enrollees, 18% are in plans where that waiver has already expired, compared to 42% who would have been in plans where these waivers would have expired by now if insurers had not reevaluated their expiration dates since July. In other words, plans covering about 24% of enrollees across all fully-insured commercial markets extended their waiver expiration dates from some point in the past to the future. As a result, plans covering 71% of enrollees in all fully-insured commercial markets continue to have COVID-19 treatment cost waivers in place at this time.
In total, 37 of the 61 insurers or parent companies we identified as having cost-sharing waivers have extended their expiration dates. Most notably, nearly half of enrollees (49%) in both markets are now in plans that have waived cost-sharing for COVID-19 treatment until the end of the year, up from about a third (31%) during our initial review. Compared to late July, a similar share of enrollees are in plans that have not specified an end date on their waivers but several more insurers have waived cost-sharing until the end of the declared national public health emergency, currently set to expire on January 20, 2020 (Inauguration Day). Most of these waivers still only apply to COVID-19 treatment received from in-network providers or facilities and consumers who are treated out-of-network may be forced to pay the entire cost of their treatment.
Included in these estimates are enrollees who live in one of the five states or the District of Columbia that mandate or have agreements with fully-funded insurers to waive cost-sharing for COVID-19 treatment, although the expiration dates of these mandates vary by state. Combined, these states account for 7% of the individual market and 9% of the fully-insured group market. Roughly 80% of enrollees in either market are in a plan that voluntarily waived cost-sharing for COVID-19 treatment at some point during the pandemic.
Premium credits
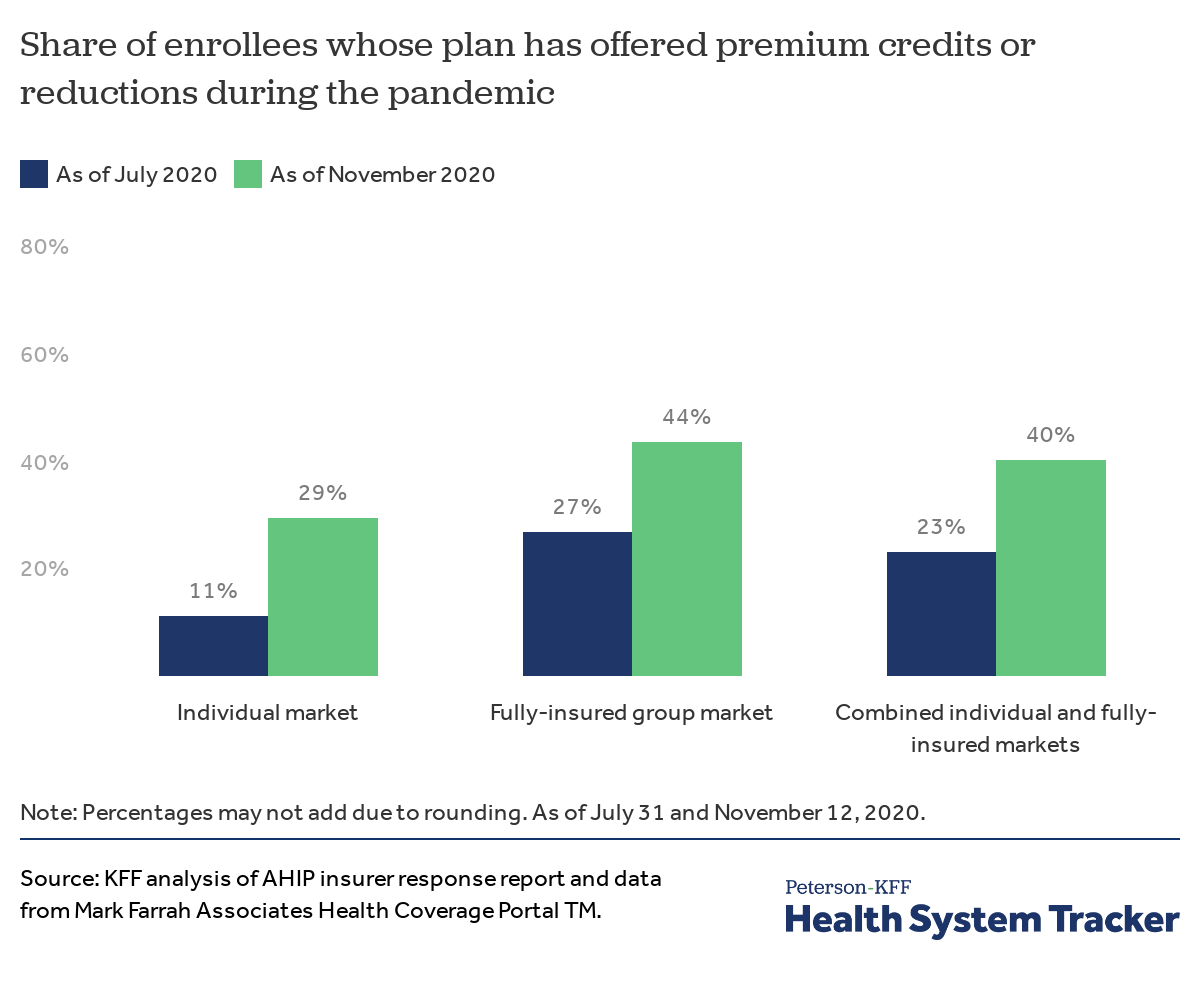
Insurers are generally not allowed to change the amount of premiums owed in the middle of a plan year; however, CMS released guidance earlier in the year allowing individual and small-group insurers to temporarily offer premiums credits to enrollees. As of late July, 11% of individual market enrollees and 27% of fully-insured group market enrollees were in plans offering some form of premium relief (credit or reduction). The chart below shows how these shares have grown, as more insurers have moved to offer premium relief in the time since.
More enrollees have experienced some form of premium relief as plans increasingly adopt such measures
Currently, 29% of individual market enrollees and 44% of fully-insured group market enrollees are in plans that have already or will soon offer premium credits. Premium credits are likely more common among fully-insured group plans because most individual market enrollees receive some form of financial assistance (i.e. Advanced Premium Tax Credits, Cost-Sharing Reductions).
Discussion
Motivated by high profits and some state requirements, many insurers have offered financial relief to their enrollees amid the coronavirus pandemic, primarily through waived COVID-19 treatment costs and less commonly through premium credits or reductions. Since we first reviewed the prevalence of these waivers and premium credits in July, many insurers have extended their waivers or newly moved to offered premium relief to their enrollees. Most cost-sharing waivers are set to expire at the end of the year or early in 2021, though it is possible that some insurers will extend these benefits once again, particularly if the national public health emergency declaration is extended next year.
Consumers who seek treatment for COVID-19 (especially those who are treated by out-of-network providers) are likely to face high costs for care, which might be even more burdensome without cost-sharing waivers for COVID-19 treatment. Importantly, 61% of covered workers are in self-insured plans that are not explicitly covered by these waivers. Self-funded employers ultimately decide whether to waive cost-sharing or not, though some insurers allow self-funded employers to opt-in to such waivers. At this time, we do not have data on how many self-funded employers have waived these costs.
Because of the substantial drop in overall healthcare utilization this year, insurers are still on-track to see considerable profits by the end of this year. This continued profitability means that, even with many waivers extended through the end of the year and more insurers offering premium credits, insurers may still owe enrollees substantial MLR rebates next year.
Methods
We reviewed a summary of private insurers responses to the pandemic, put together by America’s Health Insurance Plans (AHIP), the trade association representing private insurers. We systematically collected data from this summary as of November 12, 2020. For plans included in the AHIP summary, we merged on enrollment data as of the first quarter of 2020. Enrollment data were reported to the National Association of Insurance Commissioners (NAIC) and compiled by Mark Farrah Associated TM. State actions on cost-sharing and premium policies were sourced from KFF’s tracker of State Data and Policy Actions to Address Coronavirus, which is updated daily.
The Peterson Center on Healthcare and KFF are partnering to monitor how well the U.S. healthcare system is performing in terms of quality and cost.