Social distancing recommendations have led many health providers to increasingly deliver care through telehealth services. The precipitous increase in telehealth is in contrast to the year prior to the pandemic when relatively few enrollees utilized telehealth services. There has been tremendous interest from health care providers, regulators, and employers on how to meet the needs of patients despite disruptions arising from the pandemic. Telehealth encompasses a broad range of provider-patient communication through online portals, and audio- or video-enabled tools. Our prior analysis surveyed some of the policy and patient-level considerations that are influencing how telehealth is being adopted.
Thus far into the pandemic, governments and payers have attempted to increase access to telehealth through regulatory and payment changes. For example, Medicare began reimbursing for telehealth services in response to the COVID-19 pandemic to encourage increased utilization of telehealth. For the duration of the pandemic, Medicare is also reimbursing audio-only services for individuals in remote areas and without access to internet for video communication. The Centers for Medicare & Medicaid Services (CMS) have also incentivized private payers to cover telehealth services during the pandemic through other payment programs, such as the risk adjustment program for the individual and small group markets.
Beyond changes to payment and reimbursement policy, the continued use and expansion of telehealth services will depend on patients’ familiarity with the technology, their access to the internet, and how the availability of telehealth services is communicated to enrollees. This brief uses data from the 2019 American Community Survey (ACS) to estimate how many individuals in the U.S. had access to the internet at home in 2019. While households without internet access may have acquired access during the course of the last year, internet access prior to 2020 is suggestive of some of the disparities in individuals’ access to communication technology and might inform discussions on extending the availability of telehealth services.
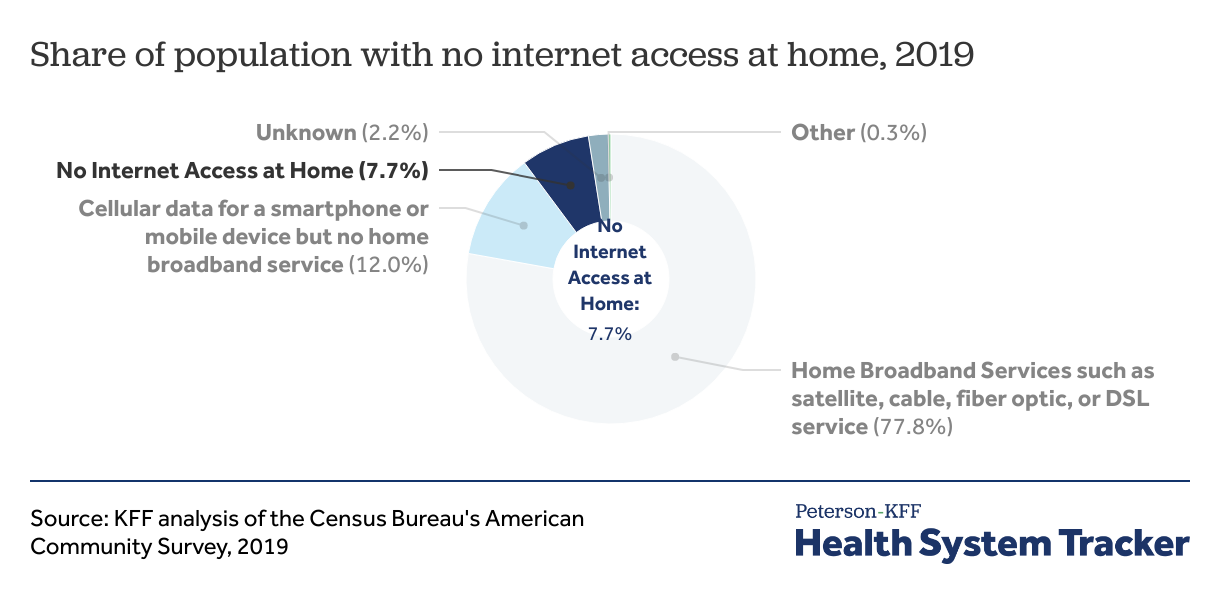
25 million Americans lack access to internet at home
25 million (8%) people in the U.S. did not have internet access at home in 2019. Across all households, 78% of Americans had access to broadband including satellite, cable, fiber optic, or DSL service connection at home. 14 million people did not have equipment capable of playing video, such as a laptop, pc computer, smartphone, tablet, or other device.
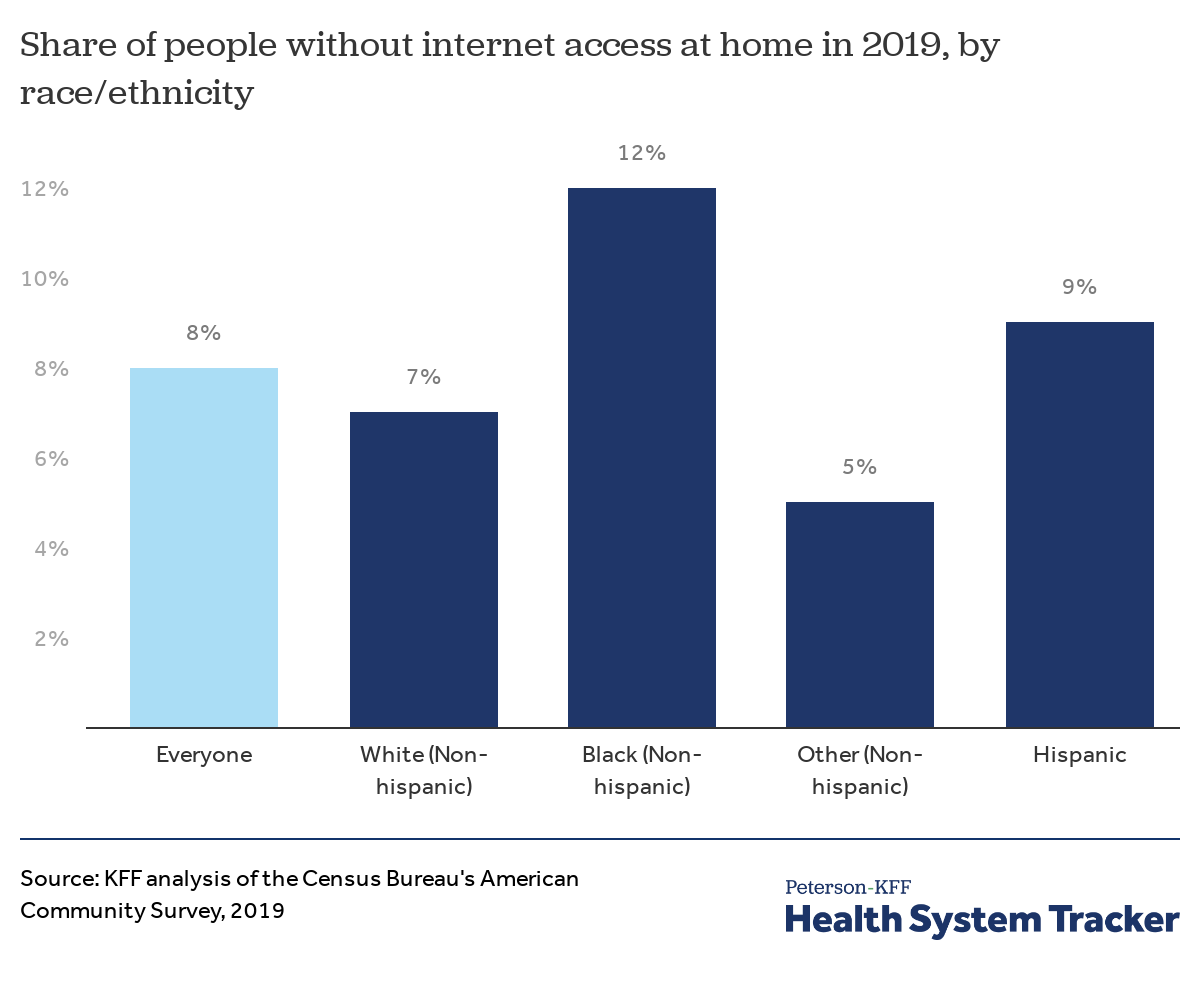
A higher proportion of Hispanic and Black Americans did not have internet access at home in 2019
A larger share of Hispanic and Black Americans did not have access to the internet at home. There were also significant differences by age, with 28% of Black seniors and 24% of Hispanics seniors lacking internet access at home (compared to 18% of all seniors).
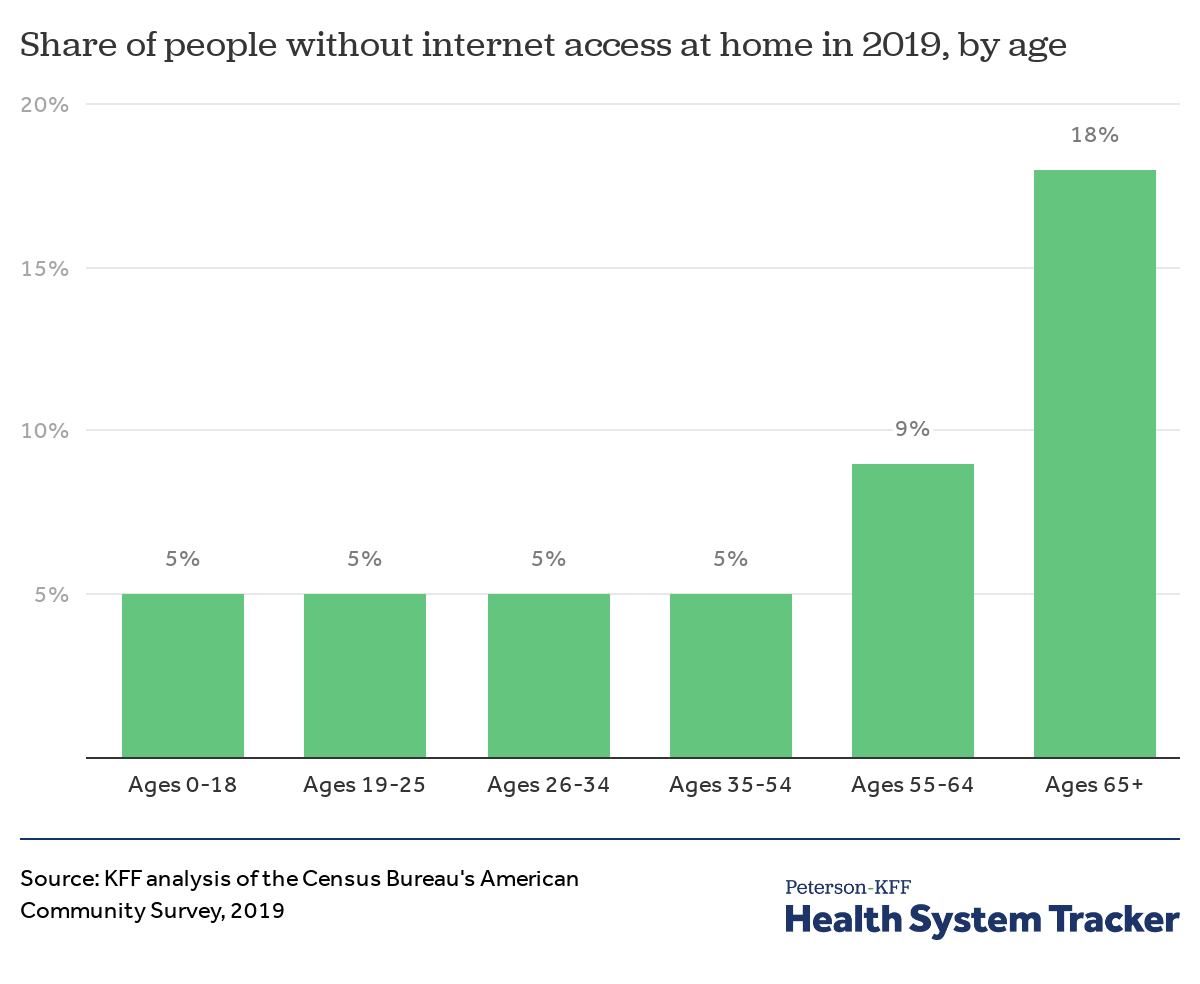
Almost 1 in 5 seniors do not have internet access at home
There were large disparities in the percent of people without internet access at home by age. Just 5% percent of people under age 55 lacked access to the internet at home in 2019. A higher share of older age groups did not have access to the internet. Among those ages 65 and over, almost 1 in 5 did not have internet access at home. That large shares of older adults lack access to telehealth services during the pandemic is concerning because older adults are at a higher risk of adverse events due to a COVID-19 infection, and also more likely to need medical services generally.
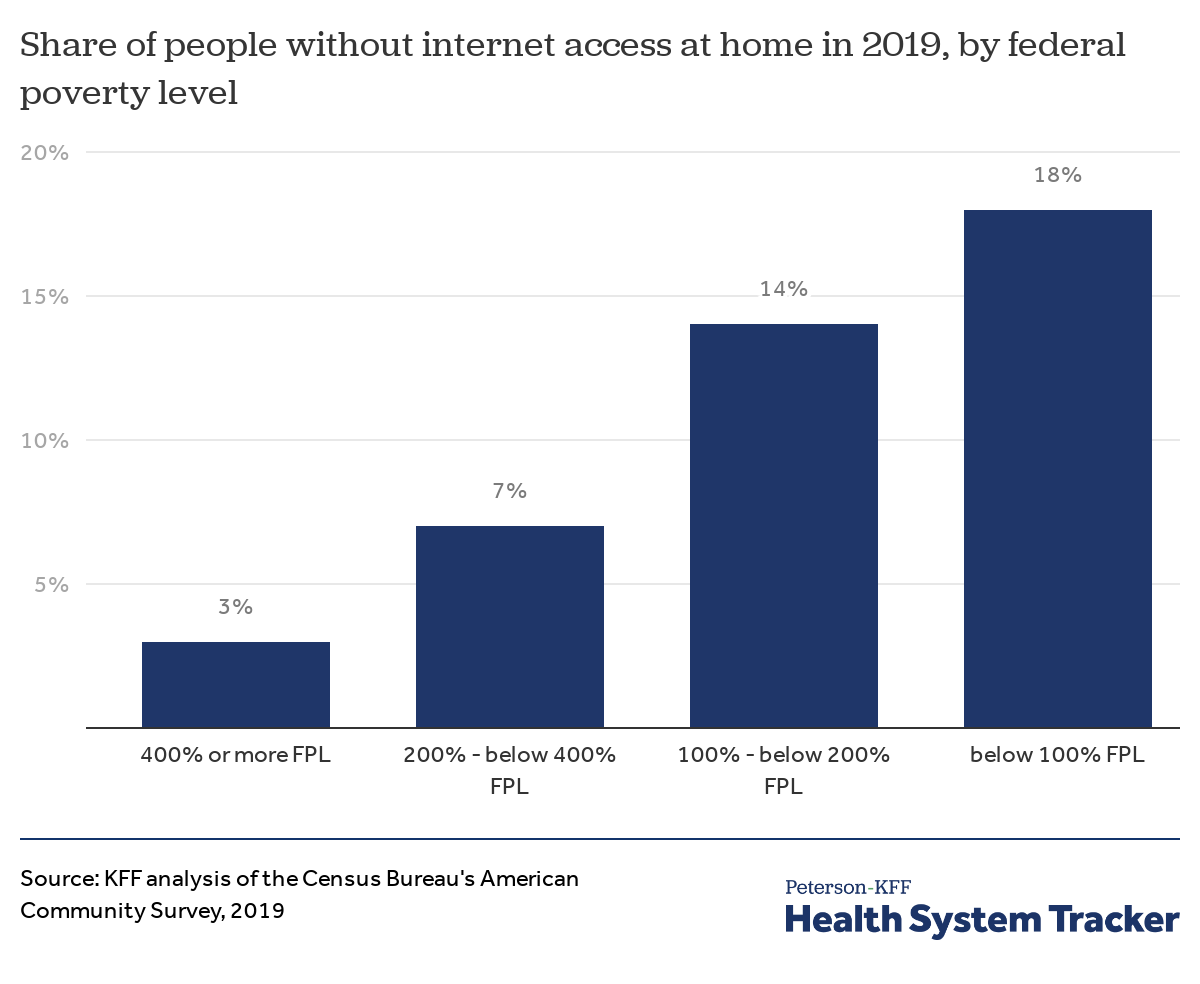
Almost 1 in 5 Americans living in poverty lack access to the internet at home
Almost 1 in 5 people with incomes below the federal poverty level (FPL) lacked internet access at home in 2019— a rate substantially higher than that of higher income Americans.
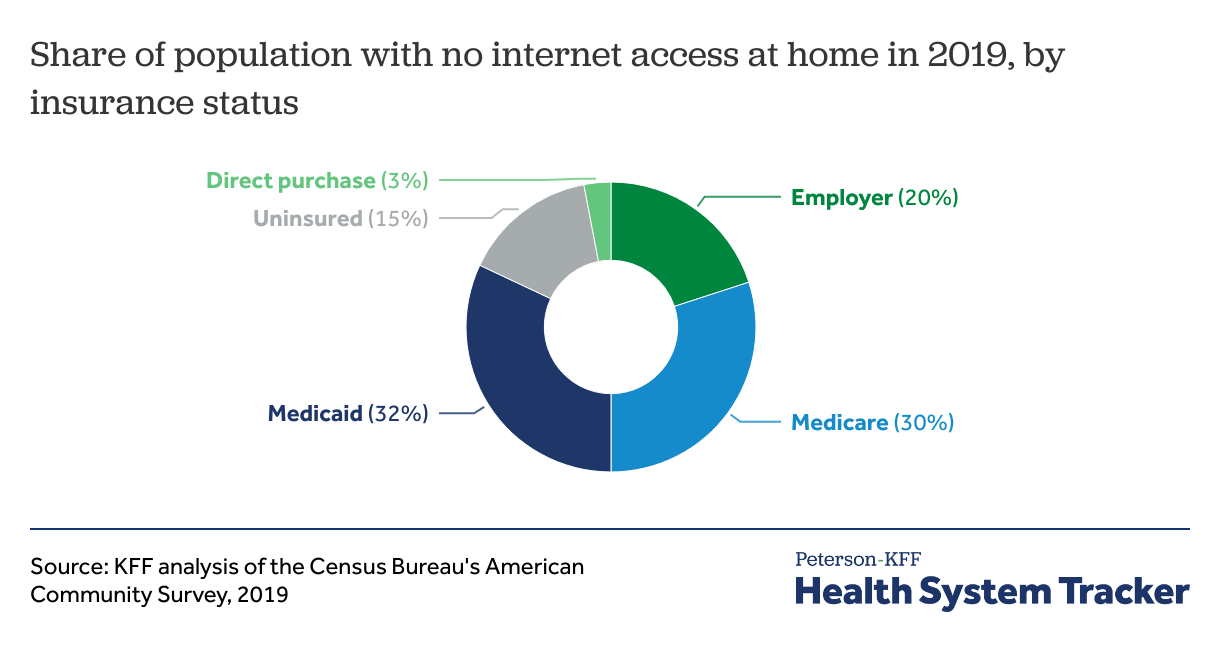
People on Medicaid and Medicare make up two-thirds of those without access to the internet at home
A higher share of people covered by public insurance programs like Medicaid or Medicare lack internet access than those insured through employers or direct purchase (individual market) plans. In all, almost 1 in 3 Americans who lack internet access at home are covered by Medicare, and a similar share are covered by Medicaid.
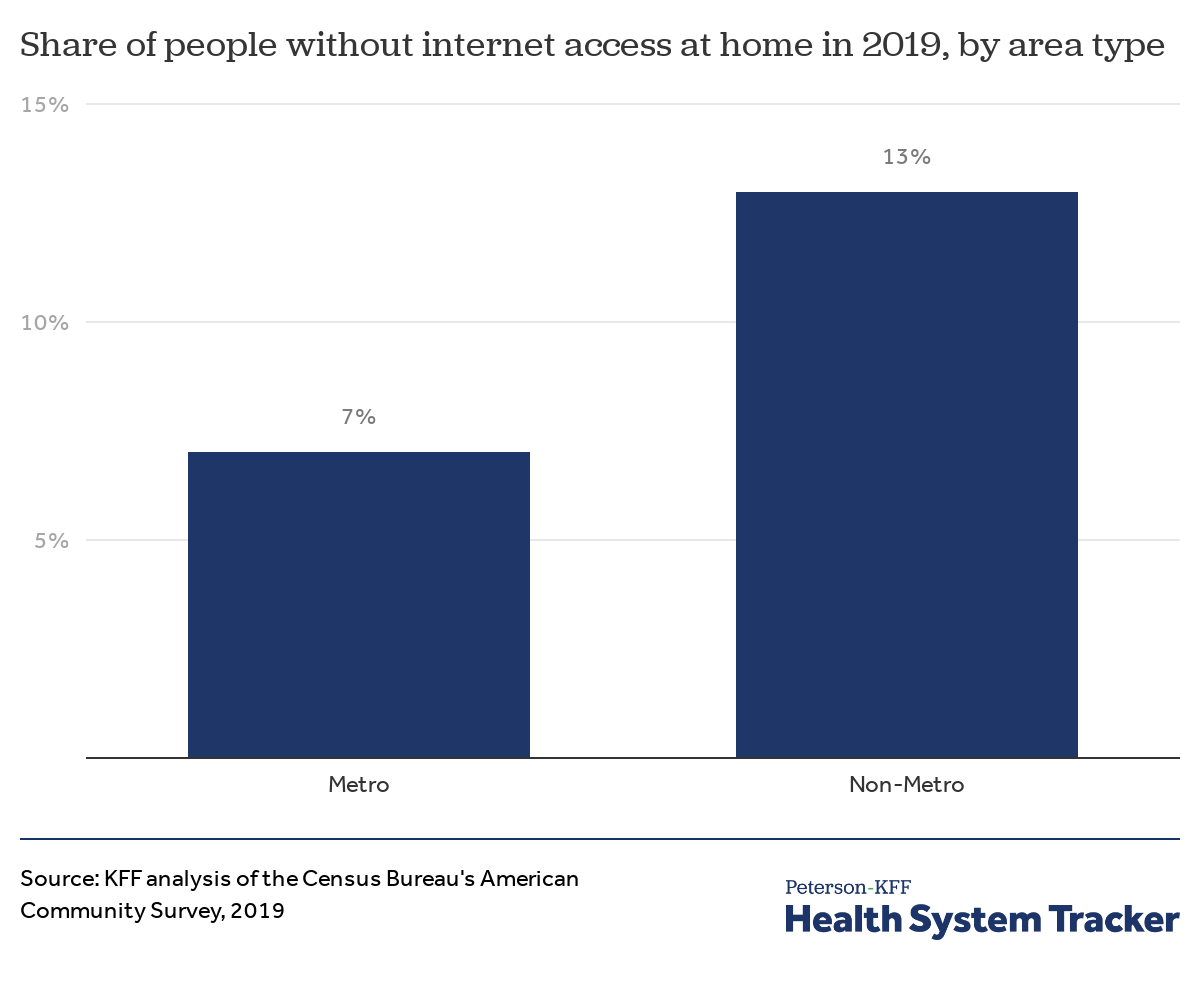
Rural Americans are almost twice as likely to lack internet access as those living in urban areas
As one might expect, internet access is more prevalent in metropolitan areas than non-metro areas with close to twice the share of the population not having access to the internet at home in non-metro areas.
Discussion
The social distancing measures implemented during COVID-19 have required many health services to be offered virtually rather than in-person. For telehealth services, internet access can be critical. However, 2019 data suggest a significant portion of Americans might not have internet access at home. Disparities in internet access across the populations may pose additional health care access concerns during the pandemic. That lack of internet access is most prevalent in rural areas and among historically underrepresented racial and ethnic groups is concerning, as this could worsen existing health care disparities. Additionally, elderly Americans may especially require access to health care services virtually while in-person care is being deferred because the elderly are at a higher risk of becoming seriously ill if infected with COVID-19 and are generally more likely to need medical services. However, nearly 20% of elderly Americans do not have internet access.
Methods
This chart collection is based on KFF’s analysis of the 2019 American Community Survey (ACS), 1-year file. The ACS includes a 1% sample of the US population. We excluded people living in noninstitutional group quarters such as college dormitories and residential treatment centers.
The ACS asks: “At this house, apartment, or mobile home – do you or any member of this household have access to the Internet?” Those who reported having internet service, with or without paying a cell phone company or internet service provider, were categorized as having access to the internet. For more information on the ACS survey questions on internet access, see here. For information on how measures of internet access may vary, see here.
We note that the share of the non-institutionalized population in the U.S. without access to the internet at home or without video-capable equipment has steadily decreased between 2016 and 2019. The share of those without access to the internet decreased by three percentage points from 11% of the population to 8% from 2016-2019. Similarly, the share of those without video-capable equipment decreased by 3% percentage points, from 7% to 4% of people. So, the share of population without access to the internet at home has likely decreased in 2020 but a substantial portion of the non-institutionalized population in the U.S. likely continues to lack access to the internet at home in 2020.
The ACS asks respondents about their health insurance coverage at the time of the survey. Respondents may report having more than one type of coverage; however, individuals are sorted into only one category of health insurance. For details on coverage type definitions, see here.
The Peterson Center on Healthcare and KFF are partnering to monitor how well the U.S. healthcare system is performing in terms of quality and cost.