COVID-19 deaths in the United States have surpassed 200,000, and the coronavirus is now the third leading cause of death in this country, after heart disease and cancer. Before the pandemic, the U.S. already had the highest overall mortality rate among similarly large and wealthy countries, and the gap has widened in the last few decades.
In this analysis, we put the pandemic’s toll into perspective by comparing where COVID-19 falls as a leading cause of death in the U.S. versus peer countries (Organisation for Economic Co-operation and Development (OECD) member nations with above median GDP and above median GDP per capita). We find that COVID-19 mortality rates are the third leading cause of death in the U.S., and COVID-19 ranks as the third highest in only one peer country, Belgium. In several peer countries (Australia, Austria, Germany, and Japan), COVID-19 is not close to breaking into the top 10 leading causes of death. Further, the U.S. nears the top of the list of countries most affected by COVID-19 on a per capita basis, surpassed only by Belgium and the United Kingdom. Finally, on a per capita basis, excess deaths this year are highest in the U.S. and the U.K. Taken together these findings suggest the pandemic will likely increase the existing mortality rate gap between the U.S. and its peers.
Leading causes of death
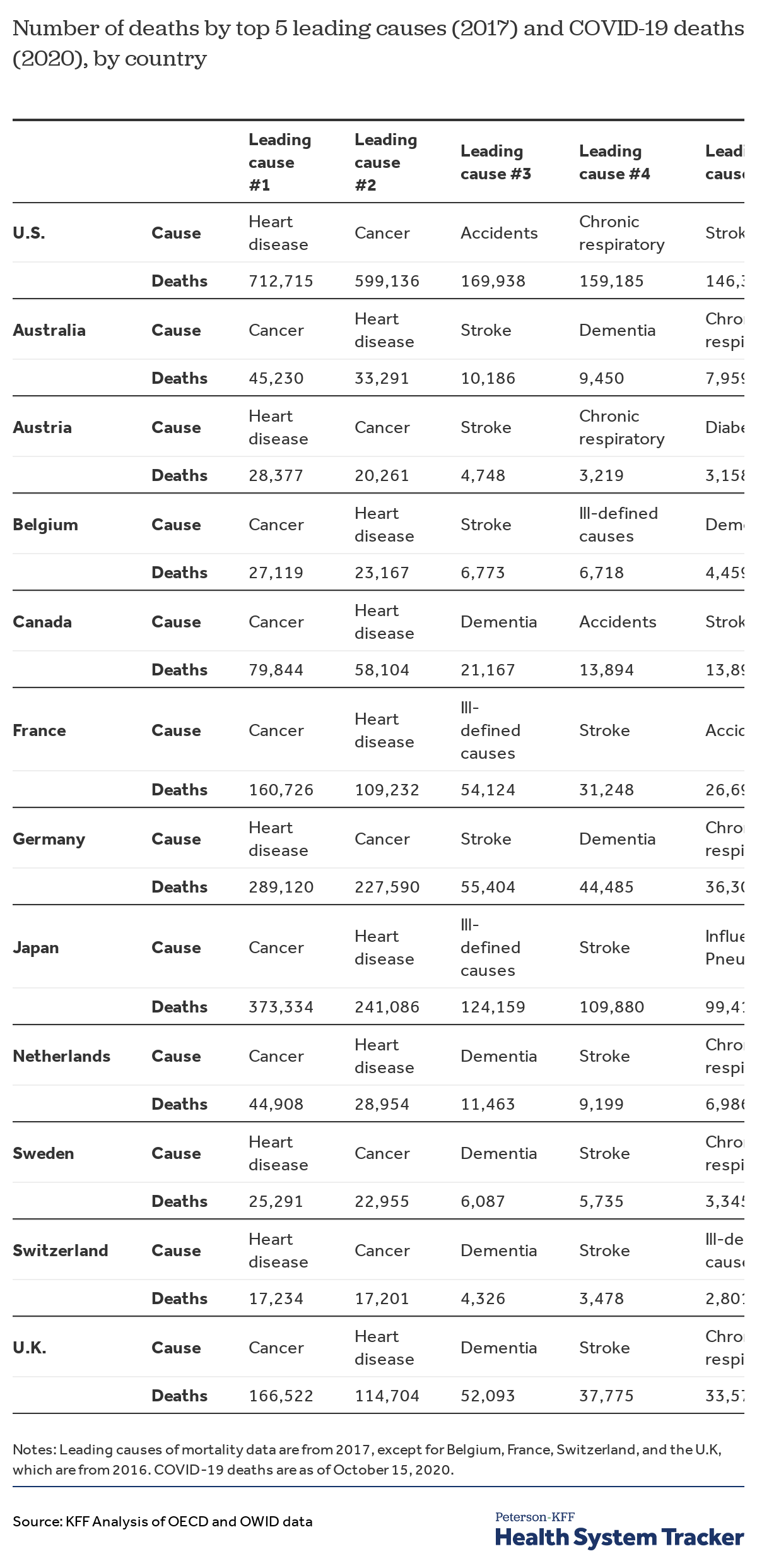
To assess where COVID-19 falls as a leading cause of death in similarly large and wealthy countries, we compared the number of deaths for the top 5 leading causes in 2017 (or the nearest data year with available data) to the number of deaths caused by COVID-19 in 2020 through October 15, 2020. Heading into the final two months of the year, we find that COVID-19 already ranks as the third leading cause of death in two of the twelve peer countries: Belgium and the U.S. In both countries, COVID-19 deaths are surpassed only by deaths due to cancer and heart disease. Although much could change in the next couple of months, in Belgium and the U.S., COVID-19 is unlikely to surpass the second leading cause of death. The ultimate ranking of COVID-19 as a leading cause of death may change in the rest of the peer countries, given that there are over two months remaining in the year.
Importantly, the pandemic may have affected mortality rates for other leading causes in 2020, which are not accounted for in these rankings. For example, deaths caused by car accidents may be lower in 2020 in places with periods of lockdown or strictly enforced social distancing. On the other hand, the pandemic could have potentially increased deaths from other causes, for example, from people delaying or not seeking care they otherwise would have.
COVID-19 reaches top causes of mortality in many countries, and has reached top 3 in the U.S. and Belgium
In three other peer countries—France, Sweden, and the United Kingdom—COVID-19 currently ranks as the fourth leading cause of death. In Sweden, COVID-19 is very close to becoming the third leading cause of death.
In Canada, the Netherlands, and Switzerland, COVID-19 has reached the top 10 leading causes of death. Meanwhile, in Australia, Austria, Germany and Japan, COVID-19 ranks 21st, 18th, 17th and 29th, respectively, out of 32 disease categories.
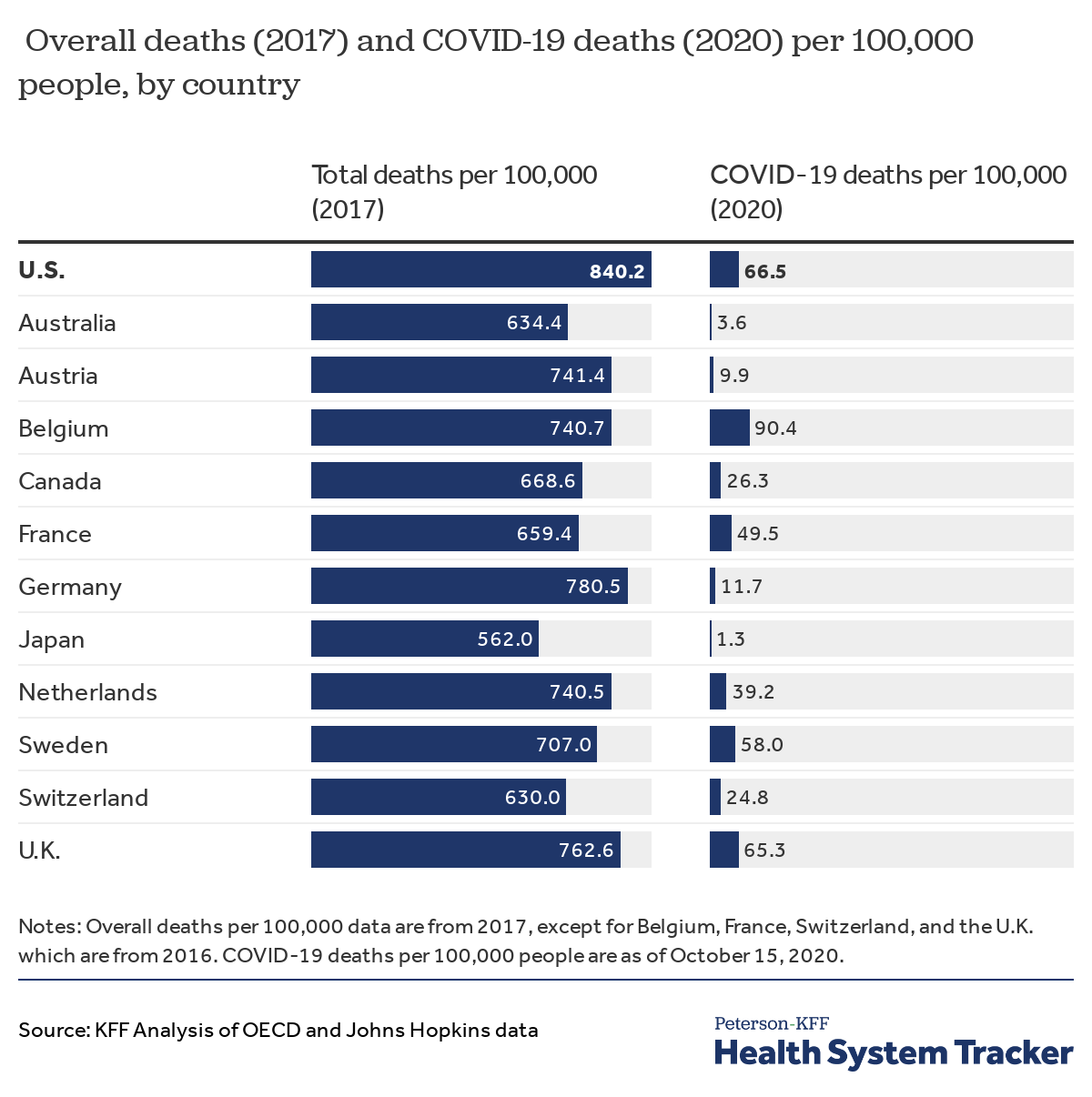
On a per capita basis, the U.S. is among the countries most affected by COVID-19 deaths
With 66.5 COVID-19 deaths per 100,000 people, the U.S. ranks second (after Belgium) on a per capita basis among comparable countries, as of October 15, 2020. Ranking by per capita COVID-19 deaths, the U.S. is firmly behind Belgium (90.4 deaths per 100,000 people) and followed closely by the U.K. and Sweden (65.3 and 58.0 deaths per 100,000 people, respectively).
By contrast, Canada has less than half as many COVID-19 deaths per capita (26.3 deaths per 100,000 people) compared to the U.S. Austria, Australia, and Japan rank as the bottom three among peer countries, with 9.9, 3.6, and 1.3 COVID-19 related deaths per 100,000 people, respectively. This shows a rather large gap between the peer countries more severely affected by the pandemic and those with lower COVID-19 mortality rates.
As seen in the overall deaths per capita, the U.S. had the highest overall death rate prior to COVID-19. The U.S. death rate per 100,000 from all causes was 840.2, compared to an average of 693.4 for peer countries in 2017. Prior to COVID-19, the U.S. had an additional 60 overall deaths per 100,000 people over the next closest country, Germany. Germany has one sixth of the number of per capita COVID-19 deaths as the U.S. so far in 2020. COVID-19 will therefore likely increase this mortality gap between the U.S. and peer countries.
Excess mortality
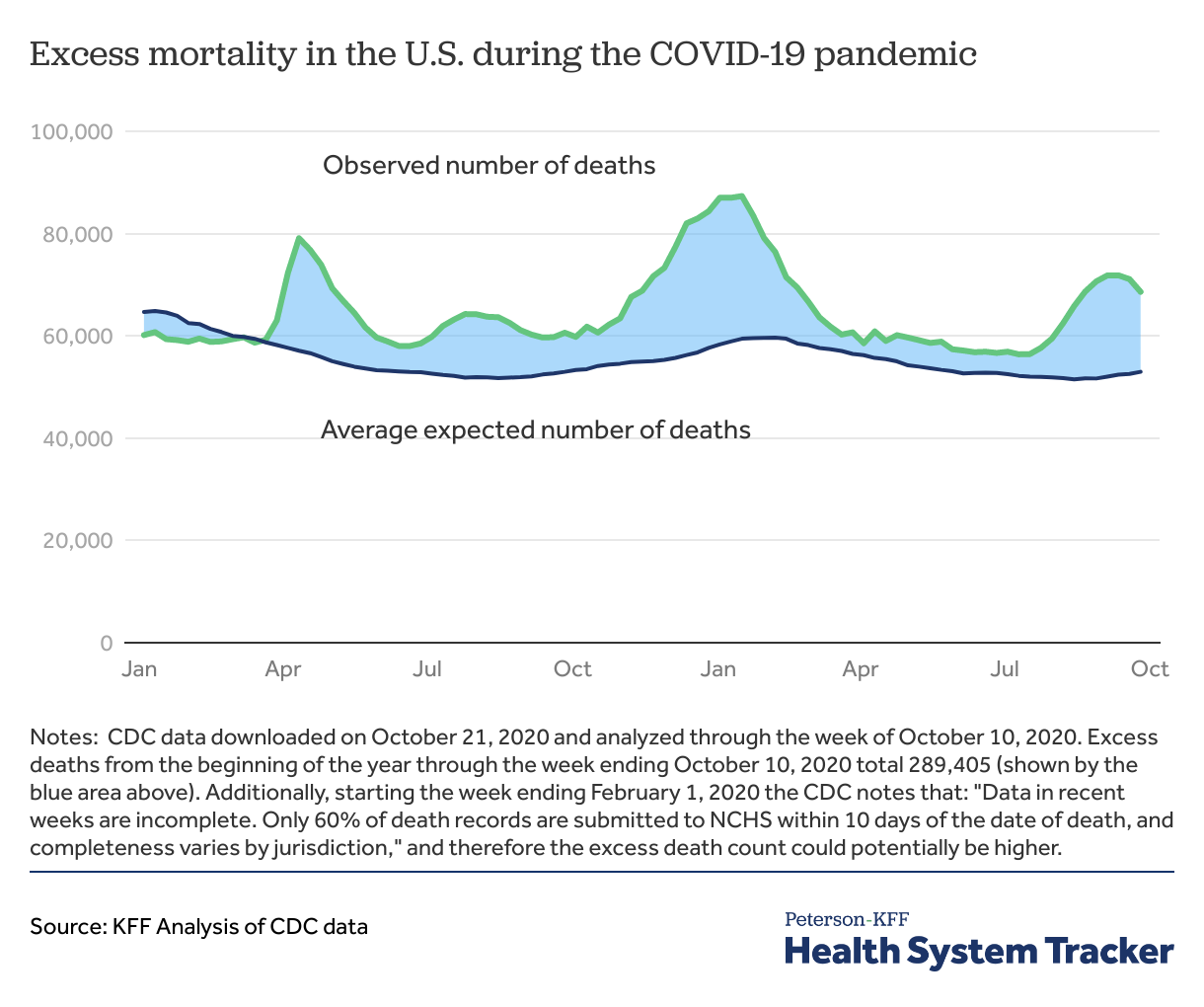
The true toll of the COVID-19 pandemic in the U.S. likely exceeds the death count attributed directly to COVID-19
During major public health crises, it can prove difficult to track down the exact number of deaths caused by the crisis directly. With limited capabilities, especially early in a pandemic, epidemiologists turn to excess deaths to put in context official death counts. Excess deaths represent the number of deaths exceeding what is expected in a typical year. This measurement serves as a good proxy for the potential mortality directly or indirectly associated with the COVID-19 pandemic.
The CDC data shows the excess deaths in the U.S. exceeds average expected number of deaths based on the prior years. Specifically, there were 289,405 excess deaths from the beginning of the year through October 10, 2020, shown by the blue area in the chart above. CDC recently published a brief on October 20, 2020, stating the high-end estimate of excess deaths totaled nearly 300,000 individuals, as of October 3, 2020. CDC also noted the deaths count attributed to COVID-19 represents two-thirds of the excess deaths count through October 3, 2020. This suggests the true toll of the pandemic might be undercounted by a large margin both due to the direct and indirect impact of COVID-19. CDC has stated that the death count from causes that could be related to COVID-19 infections have also increased in 2020 (circulatory diseases, Alzheimer disease and dementia, and respiratory diseases). So, the difference between the excess deaths and the deaths attributed to COVID-19 might be because of an undercount of COVID-19 deaths, and the indirect impact of the pandemic leading to additional fatalities, including due to delayed or foregone care.
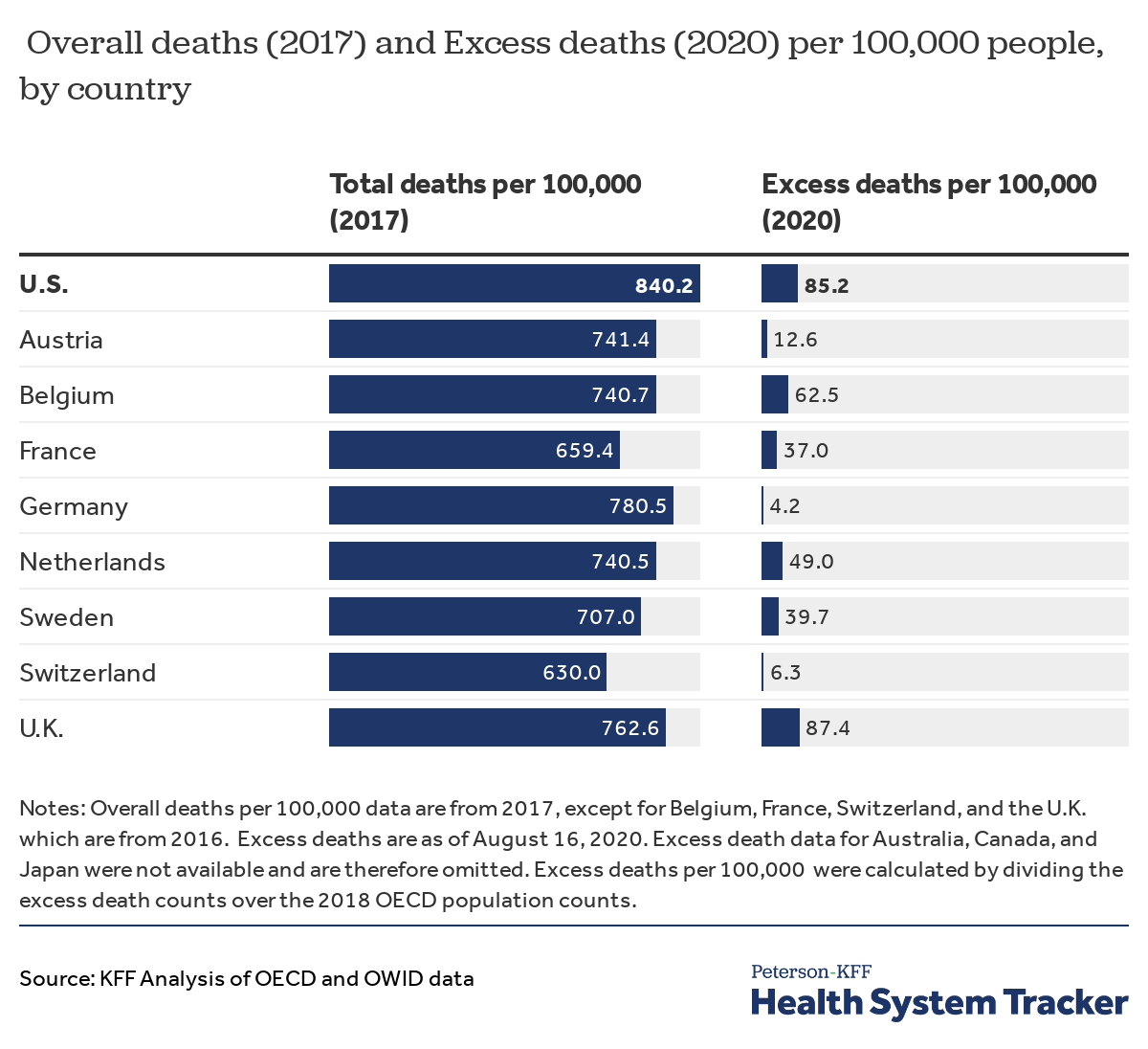
Excess death counts indicate the U.S. has been affected more severely than peer countries have been by the pandemic
The U.S.’s excess deaths count per 100,00 people is also higher than that for comparable countries. The U.S. has the second highest excess deaths count per 100,000 people at 85.2, with the U.K having the highest at 87.4 excess deaths per 100,000 people as of August 16, 2020. However, using more recent data from August 30, 2020, the U.S. has a higher rate of excess deaths per 100,000 at 90.1 than the U.K., which has 89.6 per capita. This data was not used in the chart above because not all countries reported data as of this week. As mentioned above, the U.S. already had the highest deaths per capita over peer countries, and the direct and indirect impact of COVID-19 is likely to exacerbate this mortality gap.
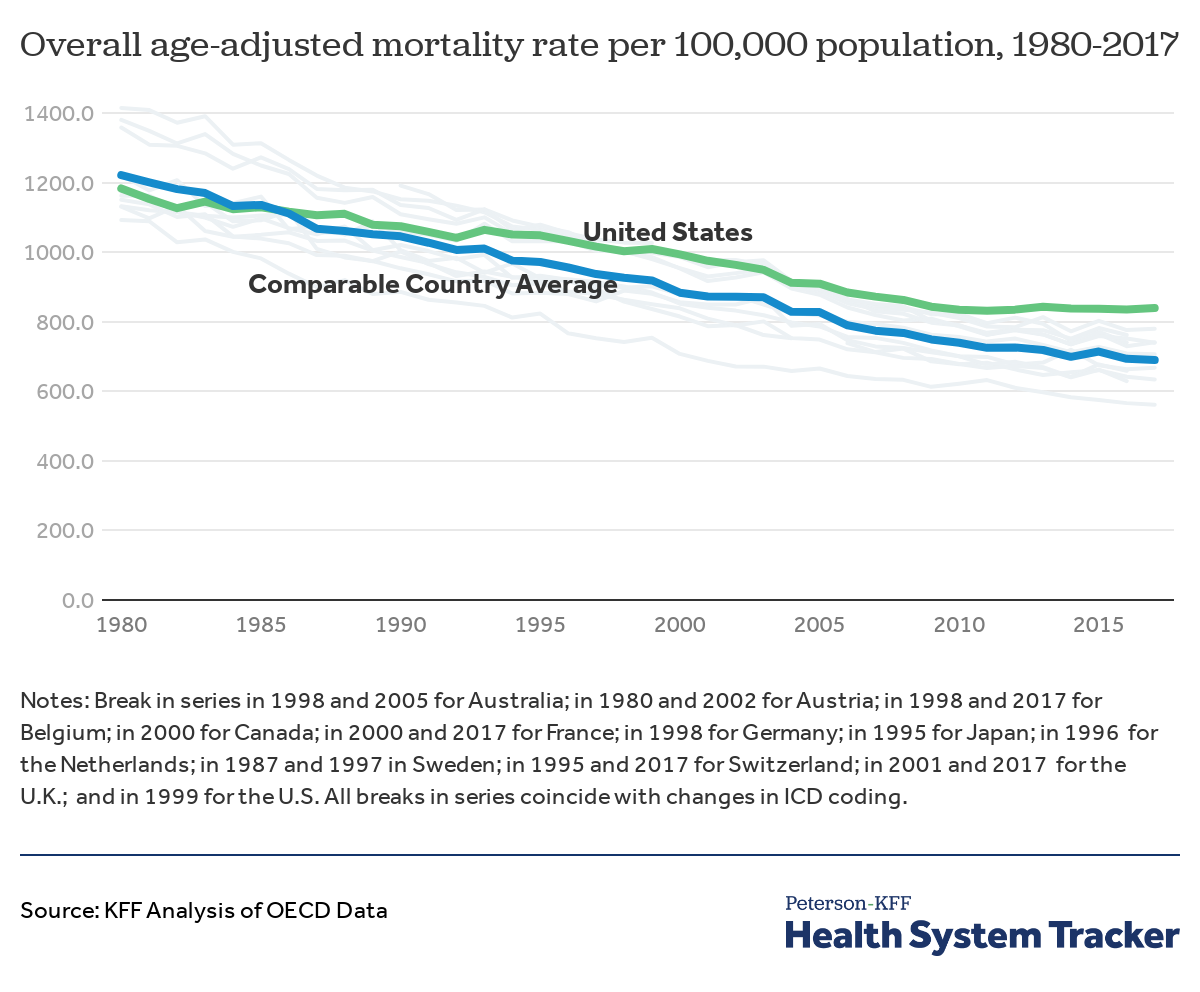
Disproportionate impact of COVID-19 on the U.S. may worsen existing mortality rate gap between the U.S. and comparable countries
The above graph shows that in recent decades the mortality rate has steadily decreased in the U.S. and in comparable countries. The U.S., however, has diverged from the comparable country averages and has had a higher mortality rate than all its peer countries even before the pandemic. While the exact degree is uncertain, it is evident that the outsized impact of the pandemic on the U.S. will likely widen the disparity in mortality and other health outcomes between the U.S. and other comparable countries.
Discussion
With over two months left in the year, the COVID-19 death count will continue to rise. This has the potential to change where COVID-19 places among leading causes of death across countries, as well as where the U.S. ranks among its peers on per capita deaths due to COVID-19. In this analysis of the pandemic’s effect on the U.S. and peer countries, we find that COVID-19 is already in the top three leading causes of death in the U.S. and Belgium; in Sweden, it is close to being in the top three as well. While COVID-19 is among the top ten leading causes of death in many peer countries, few have been affected as severely as the U.S. With higher numbers of excess deaths per capita, the outsized effect of the pandemic on the U.S. will likely widen the existing gap in mortality rates between the U.S. and peer countries.
Methods
We used the OECD Health Statistics “Causes of mortality” data from 2017 for top 5 causes of deaths. For countries where 2017 data were not unavailable, we used data from 2016. Disease grouping was done such that it was similar to the CDC’s “Deaths and Mortality” causes of death groupings. Heart disease includes all diseases of the circulatory system minus strokes, which is a separate grouping; cancer includes malignant neoplasms; and chronic respiratory includes asthma and chronic obstructive pulmonary diseases. COVID-19 death counts are derived from the Our World in Data (referred to as “OWID”) for to estimate the rank compared to other causes of death.
The COVID-19 deaths per 100,000 people data are from the Johns Hopkins Coronavirus Resource Center for the U.S. and peer countries. We used OECD Health Statistics for the overall deaths per 100,000 for 2017, or 2016 for countries where 2017 data was not available.
For the analysis showing observed deaths over those expected in 2020, we used CDC’s excess deaths data through October 10, 2020, which became available on October 21, 2020. For the comparison of excess deaths per 100,000 across countries, we used the OWID Human Mortality Database as of August 16, 2020, which is the week that all countries had data available. For each country, we divided total excess deaths by the 2018 OECD population count in order to get our excess deaths per 100,000 estimate.
When comparing between countries, we used the data as of the latest week or date available. However, we acknowledge that peer countries have differing public health infrastructures, testing capabilities, and methodology in determining what constitutes a COVID-19 related death, and that the findings in this brief are at least partially due to those differences. For example, Belgium cast a wide net in its definition of COVID-19 related deaths. Officials in Belgium have included all deaths in hospitals and care homes that are suspected but not confirmed to have been caused by COVID-19, and, as a result, it is likely that comparatively more deaths in Belgium were categorized as COVID-19 deaths than in other peer countries. In the U.S., the CDC issued guidance to use information from COVID-19 tests where possible and to report all cases where it is “probable” or “presumed” that the death was caused by COVID-19 whenever testing is not available. However, the actual approach U.S. states and counties have taken to reporting has varied significantly; most states have opted to only attribute confirmed COVID-19 deaths as such.
The Peterson Center on Healthcare and KFF are partnering to monitor how well the U.S. healthcare system is performing in terms of quality and cost.