Note: This brief was originally published on October 13, 2021 and was updated most recently in April 2022. For our analysis of COVID-19 as a leading cause of death, click here.
As of mid-April 2022, nearly 1 million people in the U.S. have died of COVID-19. COVID-19 vaccines that are free, safe, and highly effective have been widely available to all adults in the U.S. since early May 2021. Older and higher-risk adults in the U.S. had access to these vaccines months earlier. Therefore, by June 2021, adults in the U.S. could have been fully vaccinated and protected from most cases of severe illness or death due to COVID-19.
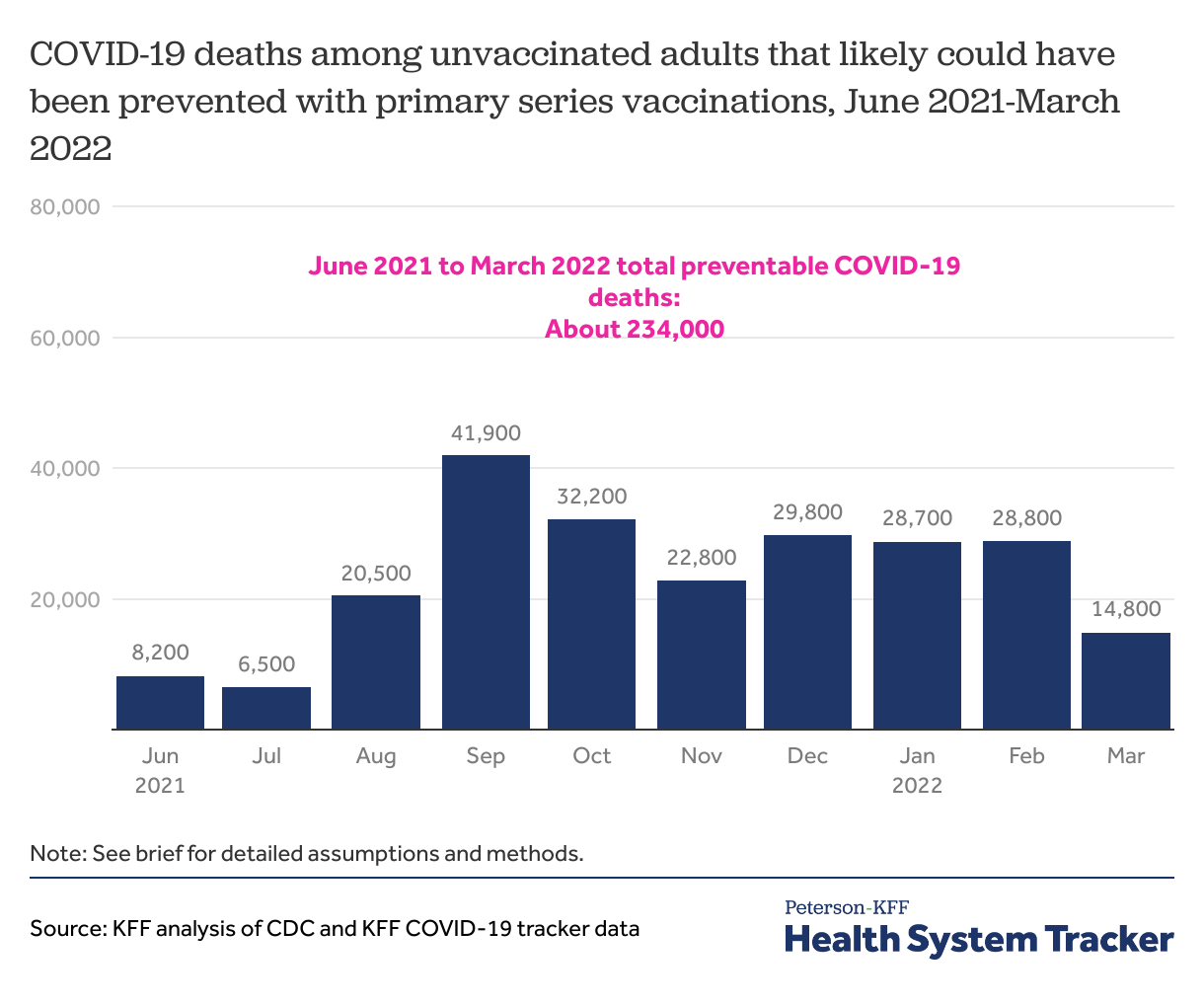
In this analysis, we estimate the number of adult deaths that could have been prevented by timely vaccination. We find that approximately 234,000 deaths since June 2021 could have been prevented with primary series vaccination. These vaccine-preventable deaths represent 60% of all adult COVID-19 deaths since June 2021, and a quarter (24%) of the nearly 1 million COVID-19 deaths since the pandemic began.
About 234,000 COVID-19 deaths since June 2021 could have been prevented with vaccinations
To estimate the number of COVID-19 deaths that could have been prevented by vaccination, we first looked at COVID-19 deaths among adults in the months after vaccines were widely available (June 2021 through March 2022). We exclude children from this analysis because vaccines have not been accessible for all children and adult permission may be required, though children represent less than 1% of COVID-19 deaths. This yields a total of about 389,000 adult COVID-19 deaths since June 2021.
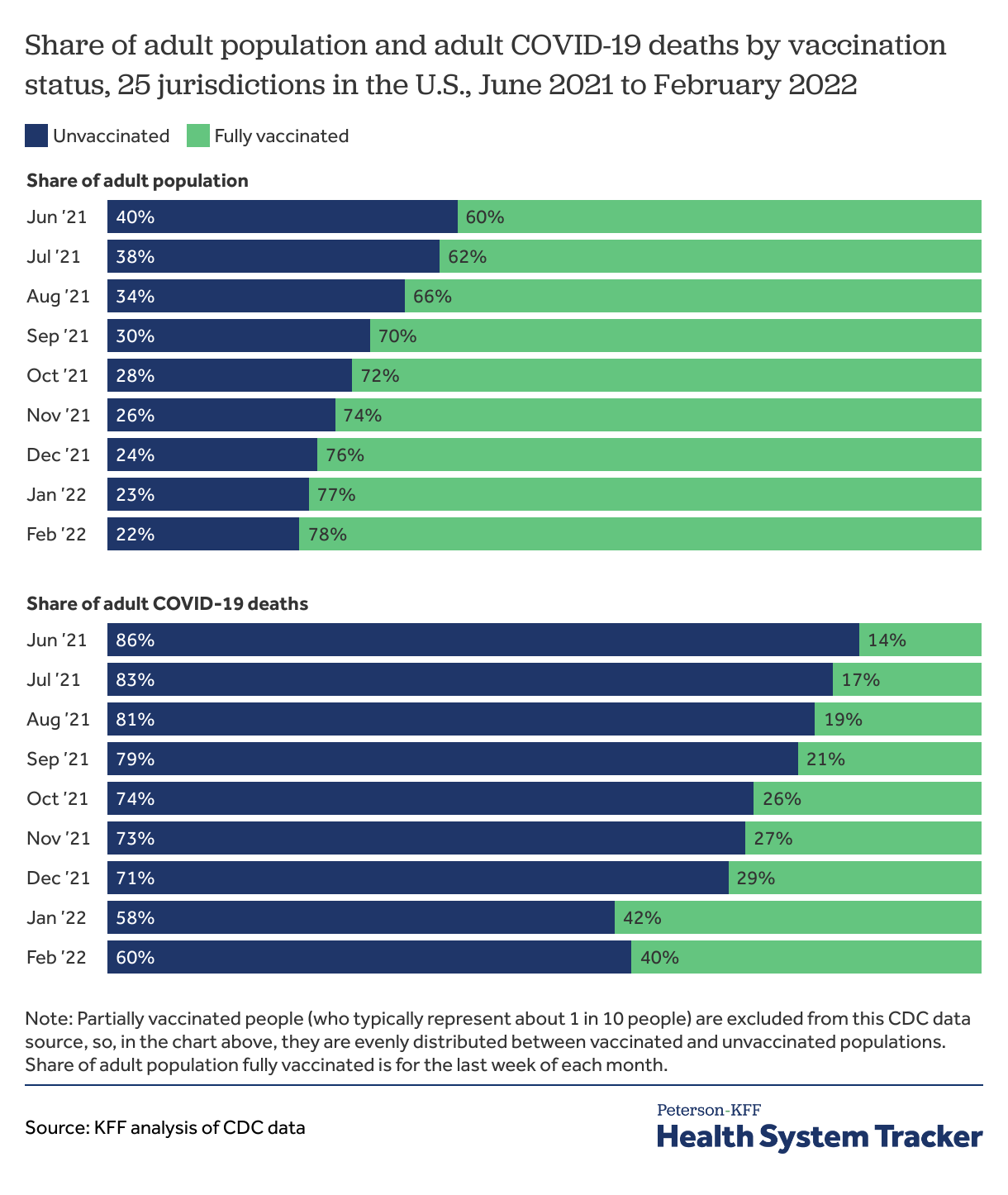
To estimate the number of deaths that could have been prevented by vaccination, we remove COVID-19 deaths among vaccinated adults from the total number of adult COVID-19 deaths in each month. Using CDC data on deaths by vaccination status for 25 jurisdictions, we calculated the share of COVID-19 deaths among those who were unvaccinated (ranging from 86% in June 2021, down to 58% in January 2022) and applied this to all adult COVID-19 deaths. We estimate a total of 270,000 adult COVID-19 deaths occurred among unvaccinated people from June 2021 through March 2022.
Unvaccinated people now represent a small share of the population, but a majority of COVID-19 deaths
Even if all of the unvaccinated adults who died of COVID-19 had chosen to get vaccinated, some of those deaths would not have been prevented with vaccination, as vaccines are not 100% effective. As described in more detail in the Methods, we use CDC studies of vaccine effectiveness for the primary vaccine series against death to estimate the number of deaths among unvaccinated adults that most likely would not have been prevented by vaccination. Because CDC estimates of vaccine effectiveness against death for the primary series have varied over time, we apply a specific vaccine effectiveness estimate by time period, ranging from 91% for June through December 2021 to 79% in January through March 2022.
While it is clear that vaccine effectiveness increases with booster shots – CDC estimates a 94% effectiveness against in-hospital death or ventilator support with a booster (third shot) – we do not estimate the potential effect of booster protection here on deaths among unvaccinated people. Had we done so, we would have found that even more unvaccinated deaths – as well as some vaccinated deaths – could have been prevented if they had not only been vaccinated, but also boosted.
Timely booster doses may have prevented additional deaths among both unvaccinated and vaccinated people
Overall, we find that from June 2021 through March 2022, approximately 234,000 lives could have been saved with a primary series of COVID-19 vaccines. These preventable deaths represent 60% of all adult COVID-19 deaths since June 2021, when vaccines became widely available, and 24% of the nearly 1 million COVID-19 deaths since the pandemic began.
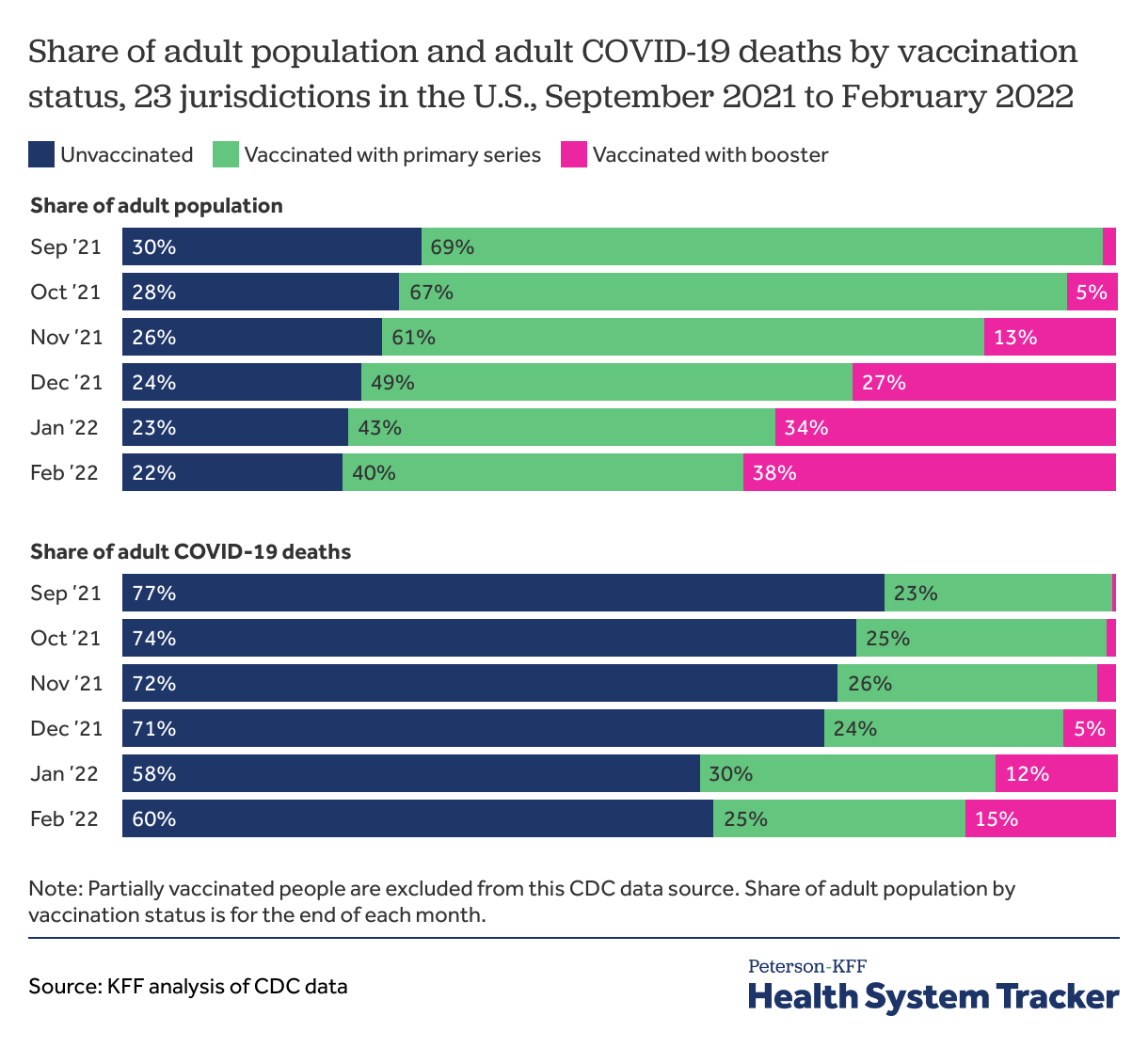
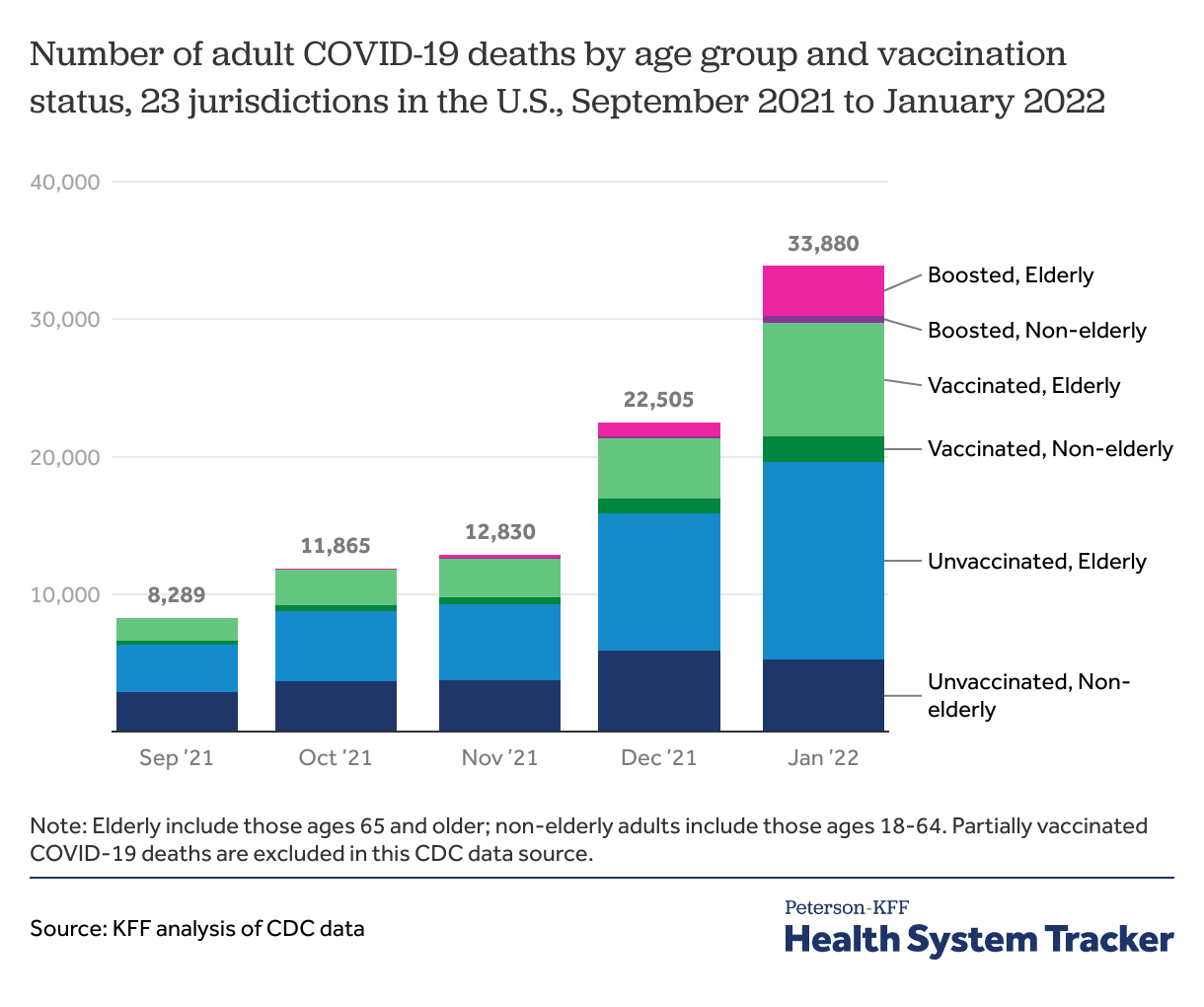
The number of deaths among vaccinated people has increased recently, particularly among the elderly, though most deaths continue to be among those who are unvaccinated
Over time, a growing share of COVID-19 deaths have occurred among people who were vaccinated, which is to be expected given that: a growing share of the adult population overall is vaccinated; immunity induced by vaccines can wane over time, which is particularly an issue for older people as they are most at risk of mortality from COVID-19 and also more likely to have been vaccinated earlier compared to younger populations; and the Omicron variant became the dominant variant in the US by the end of 2021 and has been able to evade vaccine protection against infections, especially among those without a booster dose. While currently available vaccines are substantially less effective in preventing infection with Omicron compared with earlier variants, they continue to offer significant protection against hospitalization and death, particularly for people receiving a booster dose. With many more infections, though, there was a substantial increase in the share of deaths represented by vaccinated people from December 2021 to January 2022, as Omicron took hold.
Limitations
This analysis has several limitations. First, as national data are not available for the share of deaths that are among unvaccinated people, we assume that CDC’s 25 jurisdictions are nationally representative. These jurisdictions include several large and geographically diverse states, representing 66% of the population. However, the data from the 25 jurisdictions do not include deaths among partially vaccinated people, and we are assigning deaths among partially vaccinated people equally to the “vaccinated” and “unvaccinated” groups. Partially vaccinated people typically represent about 1 in 10 people in the United States. Additionally, the 25 jurisdictions data extend through February 2022, but March 2022 data are not yet available. So, we assumed that the share of deaths that were among unvaccinated people held steady from February through March of 2022. And finally, the 25 jurisdictions data are reported based on the date of a positive specimen collection, not the date of death, but we are applying the share of vaccinated vs. unvaccinated deaths from the 25 jurisdictions data to deaths that occurred in a given month.
Another set of limitations arises with our application of vaccine effectiveness. CDC reports that earlier in the Omicron wave, vaccines (primary mRNA series without a booster dose) were 79% effective at preventing ventilator support or in-hospital death, but, to our knowledge, CDC has not yet published an estimate of vaccine effectiveness against death alone. Additionally, the vaccine effectiveness estimates we use are for the whole population, but unvaccinated people are younger, on average, and therefore vaccine effectiveness may have been different for this group compared to the adult population as a whole. We do not attempt to estimate the effect that timely booster doses may have had on preventing either unvaccinated or vaccinated deaths.
Discussion
COVID-19 vaccines continue to be highly effective against severe disease and death, even as new variants, including Omicron, have emerged. At the individual level, CDC estimates that in February and March of 2022 unvaccinated people were 10 times more likely to die from COVID-19 than people vaccinated with at least a primary series, on an age-adjusted basis. Unvaccinated people were 20 times more likely to die from COVID-19 than people with a booster dose.
Since vaccines became widely available last summer, a total of 389,000 adults in the United States have died of COVID-19, and 6 in 10 of those deaths – about 234,000 deaths – could have been prevented by timely vaccinations. This analysis underscores the importance of continued efforts to increase the number of people vaccinated and boosted against COVID-19.
These findings also have implications for vaccinated people. As noted above, a growing share of COVID-19 deaths are among vaccinated people with breakthrough infections, and many of those deaths have been concentrated in recent months during the Omicron wave and among people who did not get a booster dose. COVID-19 vaccines continue to offer tremendous protection from COVID-19 death, and that protection is significantly enhanced with recommended booster shots.
Although the focus of this analysis is on vaccine-preventable deaths, vaccines are not the only way to reduce the disease burden of COVID-19. Other precautions, such as wearing high quality masks and being in well-ventilated spaces, can also reduce risk.
Methods
In this analysis, we used the KFF COVID-19 tracker data for the number of COVID-19 deaths since June 2021 and CDC data on deaths by age groups to exclude deaths among children ages 0-17. CDC makes available a dataset based on 25 jurisdictions that shows the share of adult deaths that are among unvaccinated and vaccinated people. These data represent 66% of the total U.S. population and 57% of adult COVID-19 deaths in the U.S from June 2021 to January 2022. In these data, partially vaccinated people (those who received at least one FDA-authorized vaccine dose but did not complete a primary series at least 14 days before testing positive for COVID-19), who typically represent about 1 in 10 people, are excluded. So, in this analysis, we essentially distribute deaths among partially vaccinated people between vaccinated and unvaccinated adults. We also assume the share of deaths among unvaccinated adults in these 25 jurisdictions is similar to the national share. We applied the monthly share of COVID-19 deaths among unvaccinated adults in these data to the number of adult COVID-19 deaths nationally to arrive at an estimate of the number of COVID-19 deaths among unvaccinated adults. Since deaths by vaccination status data are not yet available for March 2022, we assume the share of deaths among unvaccinated adults was similar in March 2022 as that in February 2022 (when 60% of deaths were among unvaccinated adults), which may or may not be the case when March data become available.
Based on CDC studies, we applied a vaccine effectiveness against death of 91% from June 2021 through December 2021 and 79% for January through March 2022. Estimates of vaccine effectiveness have varied over time, and based on study populations. An early CDC study showed age-standardized vaccine effectiveness against deaths was 91% from June 20 through July 17, 2021. Another CDC study showed age-standardized vaccine effectiveness against deaths was 94% from June through November 2021. This CDC study found that from October through November 2021 (Delta wave), age-standardized vaccine effectiveness against death was 92% among fully vaccinated people with a primary series (2 doses of the Pfizer-BioNTech or Moderna mRNA vaccine or a single dose of the Janssen vaccine) and 98% among people with a booster dose. More recently, during the COVID-19 Omicron wave from December 26, 2021 to January 24, 2022, the CDC found vaccine effectiveness against ventilator support or in-hospital deaths was 79% with 2 doses and 94% with 3 doses of mRNA vaccines. Based on these studies, we use vaccine effectiveness rate of 91% from June to December 2021 and 79% from January to March 2022 to estimate the number of adult COVID-19 deaths that could have been prevented with COVID-19 vaccinations.
CDC data from 23 jurisdictions were used for charts on adult COVID-19 deaths and U.S. population that is unvaccinated, vaccinated with a primary series, or vaccinated with a booster dose. (Two of the 25 jurisdictions in the other CDC data source do not report deaths by booster status.)
Note: In a previous version of this analysis, we assumed 4% of deaths in October through November 2021 were among vaccinated people based on earlier CDC studies from June-August 2021. However, since our last analysis, CDC began publishing COVID-19 deaths by vaccination status from 25 jurisdictions for April 2021 through January 2022. In this update, we now assume 26% of deaths in October and 27% in November 2021 were among vaccinated people.
The Peterson Center on Healthcare and KFF are partnering to monitor how well the U.S. healthcare system is performing in terms of quality and cost.