The coronavirus outbreak has hit densely populated urban areas of the United States first and hardest. Some health systems have experienced surges of patients, raising concerns that there are not enough hospital beds, staffing, and equipment.
The novel coronavirus was slower to spread to rural areas in the U.S., but that appears to be changing, with new outbreaks becoming evident in less densely populated parts of the country. In this brief, we analyze variation in hospital bed capacity by region in the U.S. and by metro/non-metro status. In total, 14% of the population lives in a non-metro area. These non-metro areas are largely rural, and, even prior to the pandemic, face different challenges in health system capacity, including further travel times for patients and provider shortages. Lastly, we examine metro and non-metro differences in the share of the population that is at increased risk of COVID-19 due to age or health status.
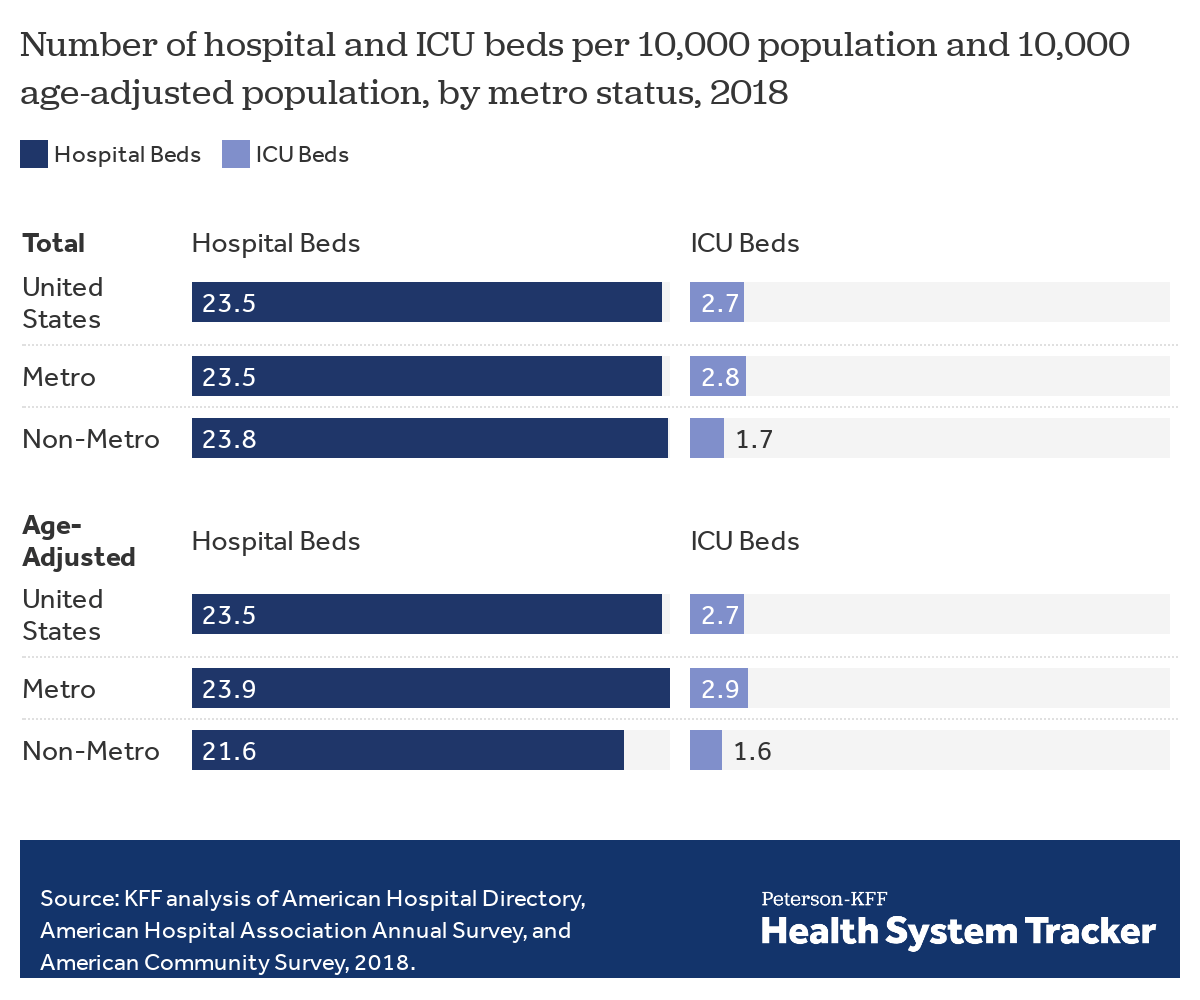
Although metro and non-metro areas have a similar number of hospital beds per capita, we find that non-metro areas have fewer ICU beds as metro areas (1.7 versus 2.8 beds per 10,000 population). Additionally, a larger share of the population living in non-metro areas are age 65 and over or have pre-existing conditions. Older adults are at increased risk of hospitalization from COVID-19 and are more likely to require intensive care. To account for the older populations in non-metro areas, we also age-adjust the number of hospital beds per capita, relative to the risk of COVID-19 hospitalization by age group (see methods for more details). After adjusting for population age, we find that differences in ICU capacity between non-metro and metro areas become more pronounced (1.6 beds per age-adjusted population vs 2.9 beds) and that non-metro areas have about 10% fewer hospital beds per age-adjusted 10,000 population (21.6) than metro areas (23.9).
If the coronavirus continues to spread in non-metro areas, these health systems could be even more strained than metro areas. While efforts such as relocating healthcare professionals and constructing temporary hospitals can alleviate some shortages, the existing capacity of hospitals will be an important factor as other parts of the country experience peak demand.
Hospital Resources Per Capita
Across the U.S., there is an average of 23.5 hospital beds and 2.7 ICU beds per 10,000 population. As shown in an earlier analysis, the U.S. has fewer hospital beds per capita than most similarly large and wealthy countries, including some other countries whose health systems have been overwhelmed by the coronavirus pandemic. One way to examine the patient capacity per hospital is by Hospital Referral Regions (HRR), which are geographic areas representing the common utilization pattern of the nation’s roughly 4,500 community, non-federal, and critical access hospitals. HRRs vary in size based on the typical distance that the population has to travel to the use hospital services.
Healthcare resources vary greatly across the U.S. Some HRRs have fewer than one ICU bed per 10,000 population, including the areas around Santa Cruz, California (0.8); Fort Collins, Colorado (0.9); Minot, North Dakota (0.9); and Wichita Falls, Texas (0.9). Meanwhile, others have more than six ICU beds per 10,000 population: Rochester, Minnesota (8.6); Colorado Springs, Colorado (7.3); Florence, South Carolina (6.9); and Tuscaloosa, Alabama (6.6).
The number of total hospital beds by HRR ranges from roughly 10 per 10,000 population in areas like Longview, Texas (9.6); Arlington, Virginia (11.6); and Mesa, Arizona (12.1) to well over 60 per 10,000 population in Grand Forks, North Dakota (86.9); Meridian, Mississippi (79.5); and Rochester, Minnesota (65.8).
For context, the Manhattan HRR, which includes the boroughs of Manhattan, Queens, Brooklyn, and Staten Island, ranks slightly above average, with 31.6 hospital beds and 2.8 ICU beds per 10,000 population, as of 2018.
Urban and Rural Differences in Hospital Resources
Of particular concern is the patient capacity of health systems in rural areas. We used the method suggested by the US Department of Agriculture to categorize metro areas as places where over half the population lives in a metro center (see Methods). We then grouped these areas by state. For example, metro Colorado includes the areas around Denver, Colorado Springs, and Grand Junction. Non-metro Colorado includes predominantly rural areas in the state.
In total, there are roughly ten times as many ICU beds located in metro areas (77,642) as in non-metro areas (7,605). On average, non-metro areas have 1.7 ICU beds per 10,000 population, compared to 2.8 beds per 10,000 population in metro areas. Non-metro areas of Colorado have 8.1 ICU beds per 10,000 population, but there is a steep decline when comparing this to the non-metro areas of other states. New Hampshire has the second highest number of ICU beds per capita in non-metro areas at 2.8 per 10,000 population, followed by South Carolina and Kentucky which both have 2.6 ICU beds per 10,000 population in non-metro areas.
The metro areas in North Dakota (6.1), D.C. (6.0), West Virginia (4.6) and Alabama (4.6) have relatively high numbers of ICU beds per 10,000 population, but metro areas in Hawaii (1.7), California (2.1), and Maryland (2.1) have closer to two ICU beds per 10,000 population.
In the case of Wyoming and New Hampshire, non-metro areas have more ICU beds per capita than metro areas. Non-metro areas of Wyoming and New Hampshire have 1.9 and 2.8 beds per 10,000 population, respectively, compared to 1.6 and 1.4 beds per 10,000 population in metro areas of the states.
The map below allows you to explore variation in total hospital bed capacity and ICU bed capacity across metro and non-metro areas, as well as how these estimates change when accounting for the age of the population.
Non-metro areas tend to have fewer ICU beds per capita than metro areas, but a similar number of hospital beds
Hospital Resources Relative to Potential Need
Older adults are more likely to require hospitalization if they become infected with coronavirus and develop COVID-19. According to data from the CDC, older adults infected with coronavirus had the highest hospitalization rate of 13.8 per 100,000 population, compared to 7.4 per 100,000 among adults ages 50 to 64 and 2.5 per 100,000 among adults ages 18 to 49. Older adults are also more likely to experience severe illness, potentially requiring intensive care and mechanical ventilation. Additionally, younger adults who have certain pre-existing conditions are also at increased risk of more severe illness if infected with coronavirus.
Non-metro areas not only have fewer ICU beds per capita on average, but also have older and sicker populations. We find that 20% of people living in non-metro areas are over age 65, compared to 15% of people living in metro areas. Using the methodology described in an earlier KFF analysis of people with illnesses putting them at increased risk if they develop COVID-19, we also find that people under age 65 living in non-metro areas are more likely to have these pre-existing health conditions (26%) than are non-elderly people living in metro areas (20%).
People living in non-metro areas tend to be older and more likely to have health conditions that put them at greater risk of COVID-19 complications
To further examine how capacity in non-metro areas compares to metro areas, we age-adjusted the population by the share of hospitalization for COVID-19. The hospital resource disparities between metro and non-metro areas in the U.S. grow larger when adjusting for population age. On an age-adjusted basis, non-metro areas have just over half as many ICU beds as metro areas, and about ten percent fewer hospitals beds. On average, metro areas have 23.9 hospital beds per 10,000 age-adjusted population, compared to 21.6 beds in non-metro areas. Metro areas have an average of 2.9 ICU beds per 10,000 age-adjusted population, compared to 1.6 ICU beds in non-metro areas in the U.S.
When adjusting for age, non-metro areas have fewer hospital beds and ICU beds
For context, the Manhattan HRR, which includes Manhattan, Queens, Brooklyn, and Staten Island, ranks relatively high with 32.7 hospital beds and 2.9 ICU beds per 10,000 age-adjusted population.
Discussion
The availability of hospital and ICU beds varies drastically across the country and within states. On average, non-metro areas of the U.S. have a similar number of inpatient hospital beds as metro areas, but fewer ICU beds. Non-metro populations are more likely to be older or have health conditions that put them at an increased risk of complications from COVID-19. When adjusting for age, compared to metro areas, non-metro areas have just over half (55%) the number of ICU beds, which are needed to care for the most severe cases of COVID-19.
If coronavirus continues to spread in rural communities across the U.S., it is possible many of these areas will face shortages of ICU beds with limited options to adapt. Patients in rural areas experiencing more severe illnesses may be transferred to hospitals with greater capacity, but if nearby urban areas are also overwhelmed, transfer may not be an option. Cities and states may increase their hospitals’ patient capacity by freeing up beds used for elective procedures or repurposing space like New York has done. However, rural areas already lacking in hospital resources and staff will have a difficult time adding capacity if they see an increase in coronavirus cases.
Methods
This brief is based on an analysis of the 2018 American Hospital Association (AHA), American Hospital Directory (AHD), the 2018 American Community Survey (ACS) data, and the Behavioral Risk Factor Surveillance System (BRFSS). Following the methodology developed by Tsai et al., the analysis includes non-federal, community, critical access hospitals.[i] In addition, hospitals in Panama City, Florida were excluded due to data irregularities. The total sum of ICU beds comes from the AHD, and includes: trauma, surgical, coronary, burn, and all general ICU beds. Neonatal, psychiatric, and pediatric ICUs were not included in the definition of ICU beds. In total, there were 4,438 hospitals included in the analysis across all 50 states and DC with over 85,000 ICU beds.
Hospital Referral Regions (HRR) are geographic areas, defined by the Dartmouth Atlas to reflect the typical referral patterns for hospitals. HRRs must contain a neurosurgical and cardiovascular surgical center, and are defined by the usage patterns of Medicare beneficiaries. Select areas of the country, such as portions of northwest Maine and southern Florida, do not have associated HRRs because the Dartmouth Atlas has labeled them as ‘not populated’ due to insufficient data. The ACS divides the United States into Public Use Microdata Areas (PUMAs), or geographic areas representing at least 100,000 people. PUMA’s vary in size based on population density. A crosswalk from the Missouri Data Center was used to map PUMAs to HRRs. In cases where a PUMA lay across multiple HRRs, all people in the HRR were assigned to the HRR with the largest share of the PUMA’s population. Population totals were calculated within HRR using the ACS.
Metro and non-metro areas are defined by the USDA Economic Research Service. Using the USDA method, 80% of the PUMAs were solely in non-metro areas, 9% contain metro areas, and 12% contained both metro and non-metro areas. The remaining PUMAs were categorized based on where the majority of the population lives. In total, 14% of the population lives in a PUMA which was classified as non-metro.
To account for differences in the age of the population, we also calculated beds per capita using age-adjusted metro and non-metro population estimates. To do so, we age-standardized the population to CDC’s estimates of the share of COVID-19 hospitalizations by age.
[i] Tsai, T., Jacobson, B., & Jha, A. (2020, March 17). American Hospital Capacity and Projected Need for COVID-19 Patient Care | Health Affairs. Health Affairs. https://www.healthaffairs.org/do/10.1377/hblog20200317.457910/full/.
The Peterson Center on Healthcare and KFF are partnering to monitor how well the U.S. healthcare system is performing in terms of quality and cost.